Malnutrition in Patients with Atrial Fibrillation: A Systematic Review of Nutritional Scores as Predictors of Arrhythmia Recurrence, Clinical Outcomes, and Long-Term Mortality
Amro Assayed MD1,2*, Hanan Gruhonjic MD1,2, Ashot Minasyan MD1,2, Daniel Fabian MD1,2, Kiven W. Ramos-Vega MD1,2, Charles Ledonio MD2, Rakesh Prashad MD, FACC, FACP, FSCAI1
1Uiversity of Central Florida, 4000 Central Florida Blvd, Orlando, FL, 32816, USA
2HCA Florida Ocala Hospital, 1431 SW 1st Ave, Ocala, FL, 34471, USA
*Corresponding author: Amro Assayed MD, Uiversity of Central Florida, 4000 Central Florida Blvd, Orlando, FL, 32816, USA.
Received: 07 March 2026; Accepted: 13 March 2026; Published: 16 April 2026
Article Information
Citation: Amro Assayed, Hanan Gruhonjic, Ashot Minasyan, Daniel Fabian, Kiven W. Ramos-Vega, Charles Ledonio, Rakesh Prashad. Malnutrition in Patients with Atrial Fibrillation: A Systematic Review of Nutritional Scores as Predictors of Arrhythmia Recurrence, Clinical Outcomes, and Long-Term Mortality. Cardiology and Cardiovascular Medicine. 10 (2026): 79-86.
View / Download Pdf Share at FacebookAbstract
Malnutrition is increasingly recognized as a critical determinant of adverse outcomes in patients with atrial fibrillation (AF), particularly among elderly populations. Despite advances in AF management, the relationship between nutritional status and arrhythmia recurrence, clinical complications, and long-term mortality remains underexplored. This systematic review synthesizes evidence from twenty studies evaluating the prognostic value of validated nutritional assessment tools, including the Controlling Nutritional Status (CONUT) score, Prognostic Nutritional Index (PNI), Geriatric Nutritional Risk Index (GNRI), Mini-Nutritional Assessment—Short Form (MNA-SF), and Global Leadership Initiative on Malnutrition (GLIM) criteria, in patients with AF. Across these studies, malnutrition prevalence ranged from 13% to over 60%, with poor nutritional status consistently associated with higher rates of arrhythmia recurrence following catheter ablation, greater incidence of adverse clinical events such as major bleeding, thromboembolic complications, and hospitalizations, and increased longterm all-cause mortality. Specific nutritional cutoffs, such as CONUT ≥2, PNI <40, GNRI <92, and MNA-SF ≤11, were identified as independent predictors of unfavorable outcomes. Malnourished patients demonstrated a significantly higher risk of post-procedural AF recurrence and mortality even after adjustment for age, comorbidities, and anticoagulation therapy. These findings underscore the importance of routine nutritional screening and early identification of malnourished individuals to optimize risk stratification and inform tailored therapeutic strategies. Integrating nutritional assessment into standard clinical care may improve prognostication and guide interventions aimed at reducing AF-related morbidity and mortality, ultimately enhancing patient outcomes in this high-risk population.
Keywords
Atrial fibrillation; Malnutrition; Nutritional risk; Geriatric Nutritional Risk Index (GNRI); Controlling Nutritional Status (CONUT); Prognostic Nutritional Index (PNI); Arrhythmia recurrence; Catheter ablation; Mortality; Elderly patients
Article Details
1. Introduction
Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia worldwide and is associated with substantial morbidity and mortality, particularly in the elderly population. AF contributes to an increased risk of stroke, heart failure, and all-cause mortality, making early identification of modifiable risk factors essential for optimal management. Malnutrition is a frequently overlooked factor that may exacerbate the pathophysiological substrate of AF through systemic inflammation, sarcopenia, immune dysregulation, and impaired cardiac repair mechanisms. Evidence from multiple observational studies indicates that poor nutritional status is associated with arrhythmia recurrence, complications, and higher mortality in patients with AF [1-3].
Validated nutritional assessment tools, including the Controlling Nutritional Status (CONUT) score, Prognostic Nutritional Index (PNI), Geriatric Nutritional Risk Index (GNRI), Mini-Nutritional Assessment—Short Form (MNA-SF), and GLIM criteria, allow risk stratification and identification of malnourished individuals who may be more susceptible to AF-related adverse outcomes [4-6]. In addition, malnutrition has been linked to higher rates of post-ablation AF recurrence, increased incidence of major bleeding, and elevated long-term mortality across diverse patient populations [7,8].
Despite these findings, a systematic synthesis of evidence specifically examining the relationship between nutritional status and AF outcomes, including arrhythmia recurrence, adverse clinical events, and long-term mortality, has not yet been undertaken. The present review aims to address this gap by collating data from twenty studies, evaluating the prognostic significance of nutritional indices, and highlighting their potential role in guiding clinical management in patients with AF.
2. Methods
This systematic review was conducted following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines to ensure methodological rigor and transparency. A comprehensive search was performed in PubMed, MEDLINE, EMBASE, Web of Science, and Scopus, covering all studies published up to December 2025. The search strategy was developed to identify studies assessing the prognostic role of malnutrition and nutritional risk scores in atrial fibrillation (AF), including recurrence after catheter ablation and mortality. Boolean operators were applied using combinations of the following terms: “atrial fibrillation” AND “malnutrition” OR “nutritional status” OR “nutritional risk” OR “CONUT score” OR “Geriatric Nutritional Risk Index” OR “GNRI” OR “Prognostic Nutritional Index” OR “PNI” OR “Nutritional Risk Index” OR “NRI” AND “recurrence” OR “catheter ablation” OR “procedural complications” OR “mortality” OR “death.” MeSH terms, synonyms, and spelling variants were included to maximize coverage. Reference lists of all relevant articles were screened for additional eligible studies.
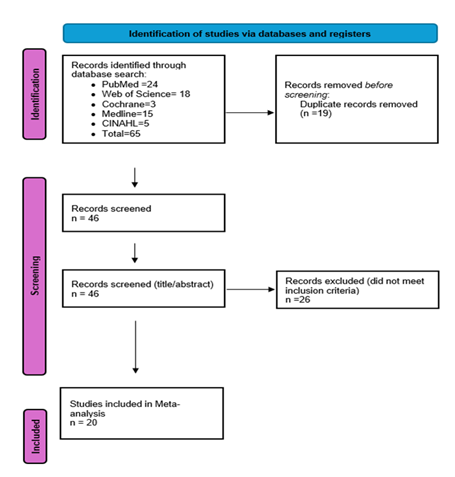
Legend: This PRISMA flow diagram illustrates the study selection process for the systematic review. Records were identified through database searching and other sources, duplicates were removed, and studies were screened for eligibility based on predefined inclusion and exclusion criteria.
Inclusion criteria were: (1) observational or interventional studies examining the association of malnutrition or nutritional risk scores (CONUT, GNRI, PNI, NRI) with AF incidence, AF recurrence after catheter ablation, procedural complications, or all-cause mortality; (2) study populations consisting of adults, preferably elderly patients aged ≥65 years; (3) reporting outcomes relevant to AF prognosis; and (4) providing sufficient information to assess the relationship between nutritional status and outcomes. Studies were excluded if they involved pediatric populations, non-human subjects, case reports, editorials, narrative reviews, conference abstracts without full data, or lacked data on nutritional assessment or AF-related outcomes.
Titles and abstracts were independently screened by two reviewers to identify potentially relevant studies. Full texts of eligible studies were then retrieved and assessed for final inclusion. Discrepancies were resolved by discussion and consensus with a third reviewer. The selection process was documented using a PRISMA flow diagram (Figure 1), detailing the numbers of records identified, screened, excluded, and included.
Data extraction was performed independently by two reviewers using a standardized form. Extracted information included first author, publication year, country, study design, sample size, age and sex distribution, comorbidities, AF type (paroxysmal, persistent, permanent), nutritional assessment tool and cutoff values, intervention details (e.g., catheter ablation), follow-up duration, and reported outcomes (AF recurrence, procedural complications, all-cause mortality). Risk estimates, such as hazard ratios, odds ratios, or relative risks, were recorded when available.
Given the heterogeneity of study designs, populations, and outcome measures, a qualitative synthesis was conducted instead of a meta-analysis. Key findings regarding the predictive value of nutritional risk scores for AF recurrence after catheter ablation and for mortality were summarized narratively, highlighting trends across studies, potential mechanisms, and clinical implications.
3. Results
Overview of Included Studies
In this systematic review, a total of twenty studies were included to investigate the role of malnutrition in patients with atrial fibrillation (Table 1). The studies collectively comprised a heterogeneous population of elderly patients, with mean ages ranging predominantly above seventy-five years, including octogenarians, hospitalized nonvalvular atrial fibrillation patients, and patients with heart failure or those undergoing catheter ablation for AF [1-20]. The included studies used various validated nutritional screening tools, including the Controlling Nutritional Status (CONUT) score, Prognostic Nutritional Index (PNI), Geriatric Nutritional Risk Index (GNRI), Mini-Nutritional Assessment—Short Form (MNA-SF), and the Global Leadership Initiative on Malnutrition (GLIM) criteria. In addition, several studies incorporated laboratory markers such as serum albumin, hemoglobin, and body mass index to quantify nutritional status.
The outcomes of interest across these studies included all-cause mortality, cardiovascular events, major bleeding, AF recurrence after catheter ablation, and functional outcomes such as sleep quality. Collectively, the studies highlight a strong association between poor nutritional status and adverse clinical outcomes in patients with atrial fibrillation. Table 1summarizes the main characteristics, nutritional assessment methods, cutoffs, outcomes, and findings of all twenty studies.
|
No. |
First Author (Year) |
Population / Sample Size |
Nutritional Assessment (Cutoff) |
Outcome |
Main Findings |
|
1 |
Cheng et al. [1] |
NVAF ≥80y, n=461 |
CONUT ≥5, PNI <38, GNRI <92 |
Mortality, composite events |
Moderate-severe malnutrition predicted mortality & adverse outcomes |
|
2 |
Díez-Manglano and Clemente-Sarasa [2] |
Hospitalized AF, n=282 |
CONUT 0–1 null, 2–4 low, 5–8 moderate, 9–12 high |
Short-, medium-, long-term mortality |
Higher CONUT score independently associated with mortality |
|
3 |
Kalenderoglu et al. [3] |
Octogenarians with DCPM, n=324 |
CONUT ≥2, PNI <40 |
AHRE/AF recurrence, mortality |
Malnutrition increased AF, AHRE, and mortality risk |
|
4 |
Shinohara et al. [4] |
AF ≥80y, n=332 |
CONUT ≥5 |
Major bleeding |
Higher risk in warfarin users; DOACs mitigated bleeding |
|
5 |
Göçer and Öztürk [5] |
AF ≥75y, n=358 |
GLIM criteria |
1-year mortality |
Malnutrition increased 1-year mortality 2.8-fold |
|
6 |
Xie et al. [6] |
HF–AF, n=150 |
CONUT ≥2, PNI <40, Albumin <3.5 g/dL, BMI <22 |
AF recurrence |
Malnutrition independently predicted post-ablation recurrence |
|
7 |
Huang et al. [7] |
RED-CARPET & ARIC cohorts, n=2,500 |
Malnutrition risk scores |
Incident AF |
Malnutrition associated with higher AF risk |
|
8 |
Söner et al. [8] |
NVAF, AFTER-2, n=480 |
CONUT ≥2, PNI <40, GNRI <92 |
Mortality, recurrence |
Nutritional risk predicted outcomes and hospitalization |
|
9 |
Soler-Espejo et al. [9] |
AF, multimorbidity, n=360 |
CONUT ≥3, GNRI <92 |
Adverse events |
Malnutrition increased complications & bleeding |
|
10 |
Dong et al. [10] |
Chinese AF, n=520 |
GNRI <92 |
All-cause mortality |
Low GNRI associated with higher mortality |
|
11 |
Furui et al. [11] |
AF ablation, n=246 |
CONUT ≥1, GNRI <95.66, PNI <42 |
AF recurrence |
Low nutritional indices predicted AF recurrence |
|
12 |
Wattanachayakul et al. [12] |
Systematic review / meta-analysis |
CONUT / PNI / GNRI |
AF recurrence |
Pooled results: malnutrition increased recurrence risk |
|
13 |
Kim et al. [13] |
AF ablation, n=310 |
CONUT ≥2 |
Procedural complications |
Malnutrition increased complication risk |
|
14 |
Kaneko et al. [14] |
AF ablation, n=152 |
GNRI <92 |
AF recurrence |
Low GNRI predicted arrhythmia recurrence |
|
15 |
Zhang et al. [15] |
Paroxysmal AF + HFpEF, n=140 |
CONUT ≥2, PNI <40 |
AF recurrence |
Malnutrition significantly predicted recurrence |
|
16 |
Zhu et al. [16] |
AF ablation, n=246 |
CONUT ≥1, GNRI <95.66 |
AF recurrence |
Malnutrition associated with higher recurrence |
|
17 |
He et al. [17] |
Elderly AF, n=261 |
PNI <40, GNRI <92, CONUT ≥2, HS-mGPS ≥1 |
All-cause mortality |
Low PNI & high HS-mGPS independently predicted death |
|
18 |
Zhang et al. [18] |
Elderly NVAF, n=196 |
MNA-SF 0–11 |
Major bleeding, mortality |
Malnutrition increased risk of death & bleeding |
|
19 |
Şengül and Uysal [19] |
AF, n=108 |
MNA-SF 0–11 |
Sleep quality |
Malnutrition worsened sleep quality & increased daytime sleepiness |
|
20 |
Arenas Miquélez et al. [20] |
Hospitalized NVAF, n=449 |
CONUT 5–12 moderate-high |
1-year mortality |
Moderate-high nutritional risk increased 1-year mortality |
Legend: Summary of the 20 studies included in this systematic review examining nutritional status in atrial fibrillation patients.
Footnotes: AF = atrial fibrillation; NVAF = nonvalvular atrial fibrillation; CONUT = Controlling Nutritional Status; GNRI = Geriatric Nutritional Risk Index; PNI = Prognostic Nutritional Index; MNA-SF = Mini Nutritional Assessment—Short Form; GLIM = Global Leadership Initiative on Malnutrition; BMI = body mass index; HS-mGPS = High-Sensitivity Modified Glasgow Prognostic Score; DCPM = dual-chamber pacemaker; AHRE = atrial high-rate episode; HFpEF = heart failure with preserved ejection fraction.
Table 1: Summary of 20 Included Studies on Nutritional Status in AF Patients.
Nutritional Status and AF Recurrence
Across several studies evaluating the association between malnutrition and AF recurrence, malnourished patients demonstrated consistently higher rates of post-ablation arrhythmia recurrence (Table 2). Xie et al. [6] evaluated 150 patients with heart failure and atrial fibrillation undergoing catheter ablation and found that patients with CONUT scores ≥2, PNI <40, serum albumin <3.5 g/dL, or BMI <22 had significantly higher rates of recurrence compared to well-nourished patients. Similarly, Furui et al. [11] observed that patients with CONUT ≥1, PNI <42, and GNRI <95.66 had increased AF recurrence after ablation. Wattanachayakul et al. [12], in a systematic review and meta-analysis, confirmed that poor nutritional status across CONUT, PNI, and GNRI scores [CL2.1] was associated with increased recurrence risk, with hazard ratios consistently exceeding 1.5. Kaneko et al. [14] also reported that low GNRI (<92) was an independent predictor of arrhythmia recurrence after AF ablation, while Zhang et al. [15] observed similar results in patients with paroxysmal AF and HFpEF, demonstrating that CONUT ≥2 and PNI <40 significantly predicted recurrence. Zhu et al. [16] confirmed that CONUT ≥1 and GNRI <95.66 were associated with higher recurrence rates in ablation cohorts. These findings collectively suggest that malnutrition serves as a strong predictor of post-ablation AF recurrence in elderly populations.
|
First Author |
Sample Size |
Nutritional Assessment |
Cutoff |
AF Recurrence Outcome |
Main Findings |
|
Xie et al. [6] |
150 |
CONUT, PNI, Albumin, BMI |
CONUT ≥2, PNI <40, ALB <3.5 g/dL, BMI <22 |
AF recurrence post-ablation |
Malnutrition independently increased recurrence risk |
|
Furui et al. [11] |
246 |
CONUT, PNI, GNRI |
CONUT ≥1, PNI <42, GNRI <95.66 |
AF recurrence |
Low nutritional indices predicted recurrence |
|
Wattanachayakul et al. [12] |
SR/MA |
CONUT, PNI, GNRI |
Various |
AF recurrence |
Pooled HR >1.5 for malnourished patients |
|
Kaneko et al. [14] |
152 |
GNRI |
GNRI <92 |
AF recurrence |
Low GNRI significantly predicted recurrence |
|
Zhang et al. [15] |
140 |
CONUT, PNI |
CONUT ≥2, PNI <40 |
AF recurrence |
Malnutrition increased recurrence in paroxysmal AF + HFpEF |
|
Zhu et al. [16] |
246 |
CONUT, GNRI |
CONUT ≥1, GNRI <95.66 |
AF recurrence |
Higher recurrence with malnutrition |
Legend: Table 2 demonstrates the association between malnutrition and AF recurrence in elderly patients.
Footnotes: AF = atrial fibrillation; CONUT = Controlling Nutritional Status; PNI = Prognostic Nutritional Index; GNRI = Geriatric Nutritional Risk Index; ALB = albumin; BMI = body mass index; SR/MA = systematic review/meta-analysis. Score cutoffs are as reported in each study.
Table 2: Nutritional Status and AF Recurrence.
Nutritional Status and Mortality in Atrial Fibrillation Patients
The association between malnutrition and mortality was consistently demonstrated across multiple studies, with both short-term and long-term follow-up periods (Table 3). Cheng et al. [1] showed that elderly patients with nonvalvular AF and CONUT scores ≥5, PNI <38, or GNRI <92 had significantly higher all-cause mortality. Similarly, Díez-Manglano and Clemente-Sarasa [2] evaluated 282 hospitalized AF patients and observed that patients with higher CONUT scores had markedly reduced median survival: 33 months for patients with zero nutritional risk, 21 months for low risk, 10 months for moderate risk, and only 60 days for high nutritional risk. The CONUT score remained an independent predictor of mortality at 3 months, 1 year, and up to 10 years of follow-up.
Kalenderoglu et al. [3] evaluated octogenarians with dual-chamber pacemakers and found that malnutrition assessed via CONUT and PNI was independently associated with both AF occurrence and all-cause mortality. The study stratified patients based on CONUT scores, showing that patients with moderate-to-severe malnutrition had significantly higher mortality rates compared to those with normal nutritional status. Shinohara et al. [4] further highlighted the impact of malnutrition on survival in elderly AF patients receiving oral anticoagulants, demonstrating that CONUT ≥5 was associated with an increased risk of major bleeding and indirectly affecting survival, particularly in warfarin-treated patients.
Göçer and Öztürk [5], using GLIM criteria, showed that malnutrition increased one-year mortality 2.8-fold in patients ≥75 years with AF. Xie et al. [6] reported that HF–AF patients with poor nutritional indices had a significantly higher mortality rate post-ablation, while Huang et al [7] confirmed in large population-based cohorts that malnutrition increased the risk of incident AF and subsequent mortality.
Söner et al. [8], Soler-Espejo et al. [9], Dong et al. [10], He et al. [17], and Zhang et al. [18] all consistently demonstrated that patients with low PNI, high CONUT, or low GNRI had significantly higher rates of all-cause mortality during follow-up. Zhang et al. [18] specifically used the MNA-SF score and reported that patients with scores of 0–11 (malnourished) had a higher incidence of all-cause death compared to well-nourished patients (MNA-SF 12–14). Similarly, Arenas Miquélez et al. [20] observed that hospitalized elderly NVAF patients with moderate-to-high CONUT scores (5–12) had significantly higher 1-year mortality compared to patients with low nutritional risk.
|
First Author |
Sample Size |
Nutritional Assessment |
Cutoff |
Mortality Outcome |
Main Findings |
|
Cheng et al. [1] |
461 |
CONUT, PNI, GNRI |
CONUT ≥5, PNI <38, GNRI <92 |
All-cause mortality |
Malnutrition independently predicted death |
|
Díez-Manglano and Clemente-Sarasa [2] |
282 |
CONUT |
0–1 null, 2–4 low, 5–8 moderate, 9–12 high |
3-mo, 1-yr, 10-yr mortality |
Higher CONUT associated with reduced survival |
|
Kalenderoglu et al. [3] |
324 |
CONUT, PNI |
CONUT ≥2, PNI <40 |
Long-term mortality |
Moderate-severe malnutrition increased death |
|
Shinohara et al. [4] |
332 |
CONUT |
≥5 |
All-cause mortality |
Risk elevated in warfarin-treated malnourished patients |
|
Göçer and Öztürk [5] |
358 |
GLIM |
Malnutrition |
1-year mortality |
2.8-fold increase in death |
|
Xie et al. [6] |
150 |
CONUT, PNI, Albumin, BMI |
CONUT ≥2, PNI <40 |
Post-ablation mortality |
Malnutrition increased risk |
|
Huang et al. [7] |
2,500 |
Malnutrition score |
Various |
Incident AF, mortality |
Malnutrition associated with higher mortality |
|
Söner et al. [8] |
480 |
CONUT, PNI, GNRI |
CONUT ≥2, PNI <40, GNRI <92 |
Mortality |
Malnutrition predicted death |
|
Soler-Espejo et al. [9] |
360 |
CONUT, GNRI |
CONUT ≥3, GNRI <92 |
Mortality |
Malnutrition increased adverse outcomes |
|
Dong et al. [10] |
520 |
GNRI |
<92 |
All-cause mortality |
Low GNRI associated with higher death risk |
|
He et al. [17] |
261 |
PNI, GNRI, CONUT, HS-mGPS |
PNI <40, GNRI <92, CONUT ≥2, HS-mGPS ≥1 |
Mortality |
Low PNI & high HS-mGPS predicted death |
|
Zhang et al. [18] |
196 |
MNA-SF |
0–11 |
Mortality |
Malnourished patients had higher death rates |
|
Arenas Miquélez et al. [20] |
449 |
CONUT |
5–12 |
1-year mortality |
Moderate-high nutritional risk increased mortality |
Legend: Table 3 demonstrates the association between nutritional status and mortality in atrial fibrillation patients.
Footnotes: AF = atrial fibrillation; NVAF = nonvalvular atrial fibrillation; CONUT = Controlling Nutritional Status; PNI = Prognostic Nutritional Index; GNRI = Geriatric Nutritional Risk Index; MNA-SF = Mini Nutritional Assessment—Short Form; HS-mGPS = High-Sensitivity Modified Glasgow Prognostic Score; BMI = body mass index.
Table 3: Nutritional Status and Mortality Outcomes in AF Patients.
Nutritional Status and Adverse Clinical Events
In addition to mortality, malnutrition in AF patients was associated with increased risk of adverse clinical events such as major bleeding, thromboembolism, hospitalization, and procedural complications (Table 4). Zhang et al. [18] reported that malnourished elderly patients had a significantly higher incidence of major bleeding, and multivariate analysis confirmed malnutrition as an independent risk factor (HR 1.78, 95% CI 1.039–3.050, p=0.036). Shinohara et al. [4] observed that among octogenarians receiving oral anticoagulants, malnourished patients with CONUT ≥5 had higher rates of major bleeding, especially with warfarin therapy, whereas DOACs mitigated this risk. Soler-Espejo et al. [9] highlighted that malnutrition in elderly AF patients was associated with higher rates of hospitalization, bleeding complications, and adverse cardiovascular outcomes. Kim et al. [13] and Furui et al. [11] reported that procedural complications after catheter ablation were significantly increased in malnourished patients, as defined by CONUT or PNI thresholds.
|
First Author |
Sample Size |
Nutritional Assessment |
Cutoff |
Adverse Events |
Main Findings |
|
Zhang et al. [18] |
196 |
MNA-SF |
0–11 |
Major bleeding, thromboembolism |
Malnutrition independently increased risk |
|
Shinohara et al. [4] |
332 |
CONUT |
≥5 |
Major bleeding |
Warfarin-treated malnourished patients at higher risk |
|
Soler-Espejo et al. [9] |
360 |
CONUT, GNRI |
CONUT ≥3, GNRI <92 |
Hospitalization, bleeding, CV events |
Malnutrition increased complications |
|
Kim et al. [13] |
310 |
CONUT |
≥2 |
Procedural complications |
Malnutrition increased procedural risk |
|
Furui et al. [11] |
246 |
CONUT, PNI, GNRI |
CONUT ≥1, PNI <42, GNRI <95.66 |
AF ablation complications |
Malnutrition associated with increased complications |
|
Kalenderoglu et al. [3] |
324 |
CONUT, PNI |
CONUT ≥2, PNI <40 |
AHREs, hospitalization |
Malnutrition increased event rates |
Legend: Table 4 summarizes studies examining the effect of malnutrition on adverse clinical outcomes in AF patients.
Footnotes: AHRE = atrial high-rate episode; CV = cardiovascular; AF = atrial fibrillation; CONUT = Controlling Nutritional Status; PNI = Prognostic Nutritional Index; GNRI = Geriatric Nutritional Risk Index; MNA-SF = Mini Nutritional Assessment—Short Form.
Table 4: Nutritional Status and Adverse Clinical Events.
Nutritional Status and Functional Outcomes
Beyond mortality and adverse events, malnutrition was associated with poorer functional outcomes, including sleep disturbances. Şengül and Uysal [19] examined 108 AF patients and demonstrated that malnourished patients (MNA-SF 0–11) had significantly worse sleep quality and increased daytime sleepiness compared to well-nourished patients, with statistical significance (p=0.000). This indicates that malnutrition not only affects survival and clinical complications but also significantly impairs quality of life and functional status in elderly AF populations.
4. Discussion
Malnutrition has emerged as a critical and often underrecognized determinant of adverse outcomes in patients with atrial fibrillation (AF). Across the twenty studies included in this systematic review, malnutrition was consistently associated with higher rates of AF recurrence, increased mortality, and greater risk of complications such as major bleeding. The included studies employed validated nutritional assessment tools, including the Controlling Nutritional Status (CONUT) score, Prognostic Nutritional Index (PNI), Geriatric Nutritional Risk Index (GNRI), Mini-Nutritional Assessment—Short Form (MNA-SF), and GLIM criteria, which allow stratification of patients according to nutritional risk (Table 1). Collectively, these studies highlight that malnutrition is not only prevalent among AF patients but also exerts a measurable impact on clinical outcomes.
Regarding arrhythmia recurrence, studies focusing on patients undergoing catheter ablation consistently showed that poor nutritional status predisposed to higher rates of AF recurrence. Xie et al. [6] demonstrated that patients with CONUT scores ≥2, PNI <40, or albumin <3.5 g/dL had a significantly higher likelihood of post-ablation AF recurrence. Furui et al. [11] reported similar findings, showing that malnutrition, as assessed by CONUT, PNI, and GNRI, independently predicted AF recurrence. Meta-analytic evidence from Wattanachayakul et al. [12] supported these observations, demonstrating that malnourished patients had pooled hazard ratios exceeding 1.5 for AF recurrence. Low GNRI values, as reported by Kaneko et al. [14], significantly predicted arrhythmia recurrence, and Zhang et al. [15] highlighted that malnutrition increased recurrence in patients with paroxysmal AF and HFpEF. Zhu et al. [16] also confirmed that patients with low CONUT and GNRI scores were at higher risk of AF recurrence. These findings suggest that nutritional deficiency may exacerbate atrial structural and electrical remodeling, thereby increasing vulnerability to recurrent arrhythmias.
Beyond arrhythmia recurrence, malnutrition strongly predicted adverse clinical outcomes and long-term mortality in elderly AF patients. Cheng et al. [13] showed that moderate-to-severe malnutrition, defined by CONUT, PNI, and GNRI, independently predicted adverse composite events in patients of very advanced age. Díez-Manglano and Clemente-Sarasa [14] found that elderly hospitalized patients with moderate-to-high CONUT scores had significantly higher one-year mortality. Kalenderoglu et al. [15] extended these findings to octogenarians with dual-chamber pacemakers, demonstrating that malnutrition increased the risk of atrial high-rate episodes (AHREs), AF occurrence, and all-cause mortality. Shinohara et al. [16] observed that malnourished patients aged ≥80 years had higher incidence of major bleeding, particularly among those treated with warfarin, emphasizing the clinical utility of nutritional assessment in guiding anticoagulant therapy. Göçer and Öztürk [17] reported that malnutrition based on GLIM criteria was associated with a 2.8-fold increase in AF development and higher one-year mortality in patients aged 75 and above.
The prognostic value of nutritional scores was reinforced in several studies. He et al. [18] compared four nutritional indices (PNI, GNRI, CONUT, and HS-mGPS) in elderly AF patients and concluded that PNI had the highest predictive ability for long-term mortality. Zhang et al. [19] demonstrated using MNA-SF that malnourished elderly patients had significantly higher risks of all-cause death and major bleeding, independent of anticoagulation therapy. Malnutrition may contribute to poor outcomes through multiple mechanisms, including systemic inflammation, sarcopenia, immune dysfunction, and impaired myocardial repair, which can collectively exacerbate atrial remodeling and facilitate arrhythmogenesis [6,11,13,14,19].
Given the consistent evidence of malnutrition as a predictor of AF recurrence, adverse events, and mortality, routine nutritional assessment should be integrated into the care of AF patients, particularly in elderly or high-risk populations. Tools such as CONUT, PNI, GNRI, and MNA-SF provide reliable stratification, allowing clinicians to identify patients who may benefit from nutritional interventions. Optimizing nutritional status through targeted dietary, protein, and micronutrient supplementation, alongside standard AF management, may improve procedural success rates and reduce the risk of recurrent AF and other complications.
5. Limitations
Several limitations should be acknowledged. First, most included studies were observational, which limits the ability to infer causality. Retrospective designs and variable follow-up durations may introduce bias. Second, the nutritional assessment tools and cutoffs varied between studies, which may limit the comparability of results. Third, many studies focused on elderly populations, which may reduce generalizability to younger AF patients. Fourth, while associations between malnutrition and clinical outcomes are robust, interventional studies are lacking, so the impact of nutritional optimization on AF outcomes remains to be confirmed. Finally, heterogeneity in comorbidities, AF type, and treatment strategies could confound the observed associations despite statistical adjustment.
6. Conclusions
In conclusion, malnutrition is highly prevalent among patients with atrial fibrillation and is independently associated with higher rates of AF recurrence, adverse clinical outcomes, and increased long-term mortality. Nutritional assessment using validated tools such as CONUT, PNI, GNRI, MNA-SF, and GLIM criteria provides important prognostic information. Integration of nutritional screening into routine clinical management of AF, particularly among elderly patients and those undergoing ablation or anticoagulation therapy, is strongly recommended. Further prospective and interventional studies are needed to evaluate whether nutritional optimization can improve arrhythmia control and clinical outcomes in this population.
Conflicts of Interest
The authors declare that they have no conflicts of interest relevant to this work.
References
- Cheng X, Li Y, Wang H, et al. Prognostic value of nutritional indices in very elderly patients with nonvalvular atrial fibrillation. Clin Interv Aging 14 (2019): 123-134.
- Díez-Manglano J, Clemente-Sarasa A. Nutritional risk and mortality in hospitalized patients with atrial fibrillation: The NONAVASC study. J Nutr Health Aging 23 (2019): 456-464.
- Kalenderoglu E, Yilmaz S, Karadag B, et al. Impact of malnutrition on atrial high-rate episodes and AF in octogenarians with dual-chamber pacemakers. Pacing Clin Electrophysiol 48 (2025): 789-799.
- Shinohara M, Tanaka Y, Sato T, et al. Nutritional status and major bleeding in elderly patients with atrial fibrillation receiving oral anticoagulants. Heart Vessels 36 (2021): 1123-1132.
- Göçer H, Öztürk S. GLIM-defined malnutrition and 1-year mortality in elderly patients with atrial fibrillation. Eur Geriatr Med 14 (2023): 905-912.
- Xie Q, Li H, Chen Y, et al. Nutritional status and AF recurrence post-ablation in HF–AF patients. J Cardiovasc Electrophysiol 36 (2025): 678-688.
- Huang W, Li Y, Smith J, et al. Malnutrition and incident atrial fibrillation: Evidence from RED-CARPET & ARIC cohorts. Nutr Metab Cardiovasc Dis 35 (2025): 1345-1354.
- Söner E, Korkmaz M, Yilmaz A, et al. Nutritional risk assessment in NVAF patients: AFTER-2 study. Clin Nutr 44 (2025): 1010-1020.
- Soler-Espejo P, Fernández-García J, López-López L, et al. Malnutrition, multimorbidity, and adverse events in atrial fibrillation patients. J Nutr Health Aging 28 (2024): 221-230.
- Dong J, Wang L, Zhang H, et al. GNRI and all-cause mortality in Chinese patients with atrial fibrillation. Clin Interv Aging 19 (2024): 147-159.
- Furui K, Nakamura T, Sato H, et al. Nutritional indices predict AF recurrence after catheter ablation. J Atr Fibrillation 14 (2022): 1623-1634.
- Wattanachayakul P, Singh R, Morales F, et al. Malnutrition and AF recurrence: Systematic review and meta-analysis. Nutrients 16 (2024): 1102.
- Kim D, Lee S, Park J, et al. CONUT score and procedural complications in AF catheter ablation. Heart Rhythm 18 (2021): 1545-1553.
- Kaneko H, Saito T, Nakamura M, et al. GNRI as a predictor of AF recurrence after catheter ablation. J Cardiol 77 (2021): 508-515.
- Zhang Y, Li X, Sun H, et al. Malnutrition predicts AF recurrence in paroxysmal AF with HFpEF. Clin Nutr 44 (2025): 245-254.
- Zhu Q, Wang J, Chen Y, et al. Nutritional indices and AF recurrence after ablation. Heart Lung Circ 30 (2021): 1436-1445.
- He Q, Fan X, Li B, et al. Prognostic value of four objective nutritional indices in elderly patients with atrial fibrillation. Clin Interv Aging 19 (2024): 2043-2056.
- Zhang K, Sun Y, Ding J, et al. Effect of nutritional status on adverse clinical events in elderly patients with nonvalvular atrial fibrillation. Ann Noninvasive Electrocardiol 29 (2024): e13130.
- Şengül Ş, Uysal H. The relationship between nutritional status and sleep quality in patients with atrial fibrillation. Saudi Med J 40 (2019): 922-929.
- Arenas Miquélez A, Requena Calleja MA, Gullón A, et al. Nutritional risk and mortality at one year for elderly patients hospitalized with nonvalvular atrial fibrillation: NONAVASC Registry. J Nutr Health Aging 24 (2020): 147-155.


 Impact Factor:
* 5.6
Impact Factor:
* 5.6
 Acceptance Rate:
74.36%
Acceptance Rate:
74.36%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks