Postoperative Ocular Outcomes Associated with Intraoperative Hypotension: A Global Matched Cohort Study
Laila Ibrahim¹*, Marina Gad El Sayed4, Mark Aziz³, Mary Aziz³, Maria Zakhary², Michael Zakhary², Rose Bishay4, Hasson Abdel4, Ibrahim Abboud4, Peter Zaki5, Jennah S. Barakat6, Kathryn I. Barakat6, Mark R. Barakat6
¹University of California San Diego, La Jolla, CA, USA.
²Chaffey College, Rancho Cucamonga, CA, USA.
³Mt. San Antonio College, Walnut, CA, USA.
4Department of Medicine, University of California Riverside, Riverside, CA, USA.
5Department of Neurosurgery, Loma Linda University, Loma Linda, CA, USA.
6Retina Macula Institute of Arizona, Scottsdale, AZ, USA.
*Corresponding Author: Laila Ibrahim, University of California San Diego, La Jolla, CA, USA.
Received: 31 March 2026; Accepted: 07 April 2026; Published: 14 April 2026
Article Information
Citation: Laila Ibrahim, Marina Gad El Sayed, Mark Aziz, Mary Aziz, Maria Zakhary, Michael Zakhary, Rose Bishay, Hasson Abdel, Ibrahim Abboud, Peter Zaki, Jennah S. Barakat, Kathryn I. Barakat, Mark R. Barakat. Postoperative Ocular Outcomes Associated with Intraoperative Hypotension: A Global Matched Cohort Study. Journal of Ophthalmology and Research. 9 (2026): 39-44.
DOI: 10.26502/fjor.2644-002400113
View / Download Pdf Share at FacebookAbstract
Purpose: To explore the possible ocular complications of intraoperative hypotension (IOH) using data from the TriNetX research platform, which provides de-identified patient records from numerous healthcare organizations worldwide.
Methods: Patients with and without IOH were identified on the TriNetX research platform using ICD-10 codes. The dataset initially included 144,130 patients with IOH and 4,912,179 patients without IOH. Propensity score matching based on sex, race, and relevant ICD-10 diagnoses (diseases of the circulatory, nervous, and respiratory systems, as well as endocrine, nutritional, and metabolic diseases) was used to create balanced groups of 139,967 patients with and without IOH. The outcomes that were evaluated included ischemic optic neuropathy, optic atrophy, retinal ischemia, retinal artery occlusion, and retinal vein occlusion after having a procedure that included the use of anesthesia. Risk ratios were calculated following propensity score matching.
Results: The risk of ischemic optic neuropathy was 0.01% in patients without IOH and 0.04% in those with IOH (RR: 2.94, 95% CI: 1.70, 5.10, p <0.0001). Optic atrophy also showed a significant association, with risks of 0.04% in patients without IOH and 0.06% in those with IOH (RR: 1.55, 95% CI: 1.11, 2.16, p=0.01). The risk of retinal artery occlusion was 0.02% for patients without IOH compared to 0.05% for those with IOH (RR: 2.60, 95% CI: 1.67, 4.05, p<0.001). Retinal ischemia was not shown to have a significant association (RR: 1.25, 95% CI: 0.59, 2.67, p=0.56), as well as retinal vein occlusion (RR: 1.41, 95% CI: 0.82, 2.44, p=0.21).
Conclusions: Patients who experience IOH have a significantly greater risk for ocular complications, supporting the need for close intraoperative monitoring and post-operative ophthalmic follow-up.
Keywords
Intraoperative hypotension; Postoperative ocular complications; Ischemic optic neuropathy; Retinal artery occlusion; Retrospective cohort study
Article Details
1. Introduction
Intraoperative hypotension (IOH) is a common occurrence during general anesthesia and is characterized by a decrease in mean arterial pressure (MAP) that can affect tissue perfusion [1]. Perfusion supports normal tissue function by ensuring that blood and nutrients reach cells through their natural vascular pathways, maintaining cellular metabolism, and overall physiological balance [2]. The reduced perfusion seen in IOH disrupts this balance and has been linked to postoperative complications that affect multiple organ systems, including the heart, kidneys, and brain [3]. Complications involving major organ systems may lead to chronic conditions that continue to affect patients after surgical recovery [4-12]. The postoperative effects of IOH may also vary depending on both its severity and duration during surgery, suggesting that even short episodes of hypotension may have significant consequences in vulnerable patient groups [5]. Although there is growing evidence linking IOH to these systemic effects, little research has explored its impact on ocular health, a domain that may be equally sensitive to fluctuations in MAP and blood pressure.
The eye is highly sensitive to changes in blood pressure as it depends on a constant blood supply in order to maintain retinal and optic nerve function [6]. A drop in MAP during surgery may reduce blood flow to these structures, compromising oxygen delivery and potentially leading to ocular complications such as optic nerve damage or the development of glaucoma [7,10]. While these events are uncommon, they can cause serious and sometimes permanent vision loss [8,11]. Previous studies on vision loss during surgery have mainly focused on surgical positioning, blood loss, or long procedure times, but the specific role of intraoperative hypotension remains unclear [9]. Further investigation into how intraoperative hypotension influences ocular health is necessary to better understand the mechanism involved and the risks that may follow.
Because the relationship between intraoperative hypotension and ocular outcomes has not been well defined, this study aims to examine how IOH may affect the eye. By using a large, multi-institutional database, we sought to determine the post-operative ocular complications associated with IOH. By quantifying these associations across diverse patient populations, this study aims to contribute to a more comprehensive understanding of the effects of IOH on the eye. Ultimately, identifying specific ocular complications of IOH that pose the greatest risk may help guide safer intraoperative blood pressure management and reduce the likelihood of vision-threatening events following surgery
2. Methods
TriNetX Clinical Data Platform:
We utilized data from the TriNetX Global Research Network, a database that provides secure access to de-identified electronic health records (EHRs) from major medical institutions worldwide, with the largest proportion based in the United States. TriNetX ensures full compliance with the Health Insurance Portability and Accountability Act (HIPAA) by organizing diagnoses under specific ICD codes and storing patient history and demographics in a fully de-identified format. This allows for large-scale, real-world evidence from millions of patients across diverse backgrounds.
Data Collection:
Patients with IOH were identified using ICD-10 codes for hypotension, including postprocedural, iatrogenic, drug-induced, orthostatic, and unspecified hypotension. Patients without IOH were required to have no documented hypotension diagnoses. A 1:1 nearest-neighbor propensity score matching algorithm was used to balance the cohorts based on sex and race.
Retinal artery occlusion was identified using ICD-10 codes H34.1 (central retinal artery occlusion) and H34.23 (retinal artery branch occlusion).
Retinal vein occlusion was identified using ICD-10 codes H34.81 (central retinal vein occlusion), H34.82 (venous engorgement), and H34.83 (tributary branch retinal vein occlusion) and its subcodes H34.831-H34.839.
Data Analysis:
Statistical analyses were completed using the built-in tools within the TriNetX platform. Risk ratios (RRs) with 95% confidence intervals (CIs) were calculated to assess the association between IOH and postoperative ocular outcomes. Statistical significance was defined as p-value <0.05.
Propensity score matching (PSM) was used to reduce baseline differences between patients with and without IOH. A 1:1 nearest-neighbor matching algorithm was applied, which incorporated sex, race, and various ICD-10 diagnoses that include diseases of the circulatory, nervous, and respiratory systems, as well as endocrine, nutritional, and metabolic diseases.
Ethics
As this study was performed entirely on de-identified data on the TriNetX platform, it was determined not to meet the federal definition of human subjects research [DHHS 45 CFR46.102(e), 46.102(l)] or clinical investigation [FDA 21 CFR 50.3(c), 56.102(c)] by the University of California Riverside Office of Research Integrity and the University of California, Riverside IRB, and thus exempt from further ethics review.
3. Results
A total of 144,130 patients who experienced intraoperative hypotension and 4,912,179 patients without intraoperative hypotension were identified. After 1:1 propensity score matching, 139,967 matched pairs were included in the final analysis, with baseline demographic and clinical characteristics well balanced between cohorts.
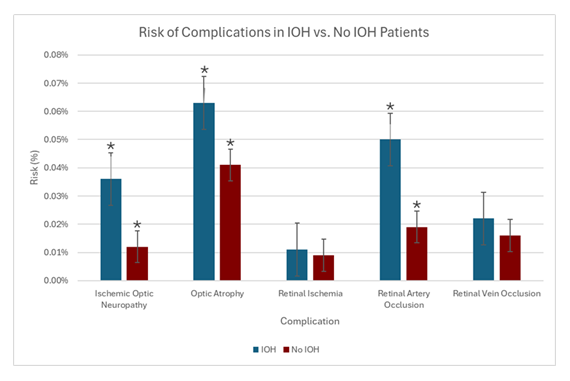
Overall, intraoperative hypotension was associated with an increased risk of several postoperative ocular complications. Patients with intraoperative hypotension demonstrated a higher risk of ischemic optic neuropathy compared with patients without intraoperative hypotension (0.04% vs 0.01%, p < 0.0001). Similarly, optic atrophy occurred more frequently in the intraoperative hypotension cohort (0.06% vs 0.04%, p = 0.01). Retinal artery occlusion was also more common among patients with intraoperative hypotension, with an observed risk of 0.05% compared to 0.02% in patients without intraoperative hypotension (p < 0.001). Absolute risk differences between groups are illustrated in Figure 1.
In contrast, no statistically significant association was observed between intraoperative hypotension and retinal ischemia (p = 0.56) or retinal vein occlusion (p = 0.21), with similar risks observed between cohorts (Figure 1)
Figure 1: Comparison of postoperative ocular complication risk between patients with intraoperative hypotension (IOH) and those without IOH following propensity score matching. Bars represent the percentage risk of each ocular outcome, with error bars indicating 95% confidence intervals. Asterisks denote statistically significant differences between groups (p < 0.05). Patients with intraoperative hypotension demonstrated higher risk of ischemic optic neuropathy, optic atrophy, and retinal artery occlusion compared with patients without intraoperative hypotension, while no significant differences were observed for retinal ischemia or retinal vein occlusion.
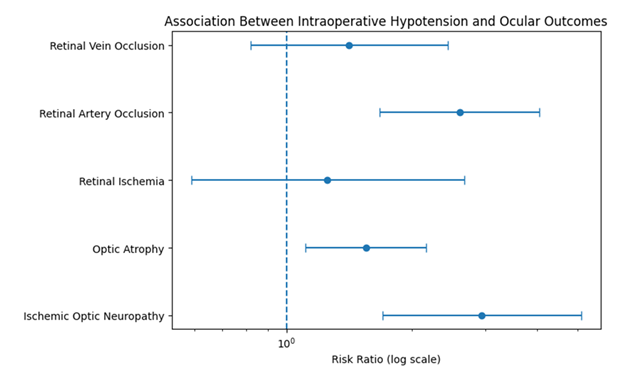
Effect estimates, using risk ratios with 95% confidence intervals, are summarized in Table 1. A forest plot depicting the relative risk estimates for postoperative ocular outcomes associated with intraoperative hypotension is shown in Figure 2, demonstrating statistically significant associations for ischemic optic neuropathy, optic atrophy, and retinal artery occlusion, while confidence intervals for retinal ischemia and retinal vein occlusion crossed the null value.
Table 1: Association between intraoperative hypotension and postoperative ocular outcomes in a propensity score–matched cohort.
|
Outcome |
IOH n/N (%) |
No IOH n/N (%) |
RR (95% CI) |
p-value |
|
Ischemic Optic Neuropathy |
50 / 139,951 (0.04%) |
17 / 139,770 (0.01%) |
2.94 (1.70–5.10) |
< 0.0001 |
|
Optic Atrophy |
88 / 138,809 (0.06%) |
57 / 139,188 (0.04%) |
1.55 (1.11–2.16) |
0.01 |
|
Retinal Ischemia |
15 / 139,810 (0.01%) |
12 / 139,897 (0.01%) |
1.25 (0.59–2.67) |
0.56 |
|
Retinal Artery Occlusion |
70 / 139,155 (0.05%) |
27 / 139,564 (0.02%) |
2.60 (1.67–4.05) |
< 0.0001 |
|
Retinal Vein Occlusion |
31 / 139,247 (0.02%) |
31 / 139,540 (0.02%) |
1.41 (0.82–2.44) |
0.21 |
Values are reported as n/N (%). RR = risk ratio; CI = confidence interval; IOH = intraoperative hypotension.
Figure 2: Forest plot illustrating the association between intraoperative hypotension and postoperative ocular outcomes following propensity score matching. Risk ratios (RRs) with 95% confidence intervals (CIs) are shown on a logarithmic scale for each outcome. The vertical dashed line represents the null value (RR = 1.0). Outcomes with confidence intervals that do not cross the null line indicate a statistically significant association with intraoperative hypotension.
4. Discussion
In this large retrospective cohort study, intraoperative hypotension (IOH) was associated with an increased risk of select postoperative ocular complications. After propensity score matching, patients with IOH displayed higher risk for ischemic optic neuropathy, optic atrophy, and retinal artery occlusion in comparison to patients without IOH, while no significant association was found for retinal ischemia or retinal vein occlusion. These findings suggest that intraoperative blood pressure instability may differentially affect ocular structures, particularly those involving the optic nerve.
Previous studies examining postoperative visual complications have primarily focused on factors such as surgical positioning, blood loss, prolonged operative duration, and patient comorbidities [9]. In contrast, the role of intraoperative hypotension has been less well characterized, particularly with respect to specific ocular outcomes. While IOH has been widely associated with adverse systemic outcomes involving the heart, kidneys, and brain, its relationship with postoperative ocular complications has not been extensively evaluated in large, multi-institutional cohorts [3].
The optic nerve is particularly vulnerable to reductions in perfusion due to its limited collateral blood supply and its tendency to become hypoxic when perfusion pressure falls below normal levels [13]. Transient decreases in systemic blood pressure during surgery may compromise optic nerve perfusion, increasing susceptibility to ischemic injury [14]. In contrast, the retina’s unique vascular architecture and autoregulatory capacity may buffer brief reductions in perfusion, which could help explain the lack of significant association observed for retinal ischemia in this study [15].
From a clinical perspective, these findings highlight the importance of maintaining hemodynamic stability during surgery, particularly in patients who may be at increased risk for optic nerve-related complications. Although postoperative ocular events remain rare, the potential for permanent vision loss underscores the need for careful intraoperative blood pressure management and heightened awareness of ocular risk factors.
In conclusion, this study demonstrates an association between intraoperative hypotension and specific postoperative ocular complications within a large, matched cohort. Further prospective studies are needed to better characterize the relationship between blood pressure management and ocular outcomes and to identify patients at greatest risk for vision-threatening events.
5. Limitations
This study has several limitations, including its retrospective design and reliance on data from the TriNetX platform, which may introduce bias related to variability in coding and documentation across institutions and limit the generalizability of these findings. The use of electronic health record data may result in incomplete or inaccurate documentation of intraoperative hypotension and postoperative ocular outcomes, and IOH was identified using ICD-10 diagnostic codes rather than direct intraoperative blood pressure measurements, limiting assessment of the severity, duration, and timing of hypotensive episodes. Postoperative ocular complications were similarly identified through coded diagnoses rather than standardized ophthalmologic examinations, which may contribute to underreporting of rare events. TriNetX anonymizes patient data by replacing event counts between 1 and 10 with a value of “10” to protect patient privacy. Although this approach can limit detailed statistical analysis of uncommon outcomes, no outcome counts in the present study fell within this range. The study also did not account for surgical complexity, anesthetic technique, or intraoperative management strategies that may influence both blood pressure and ocular risk. Despite these limitations, this study leverages a large, multi-institutional dataset to provide novel insight into the association between intraoperative hypotension and postoperative ocular complications.
Funding:
None.
Conflicts of Interest:
MRB: Consultant: AbbVie Inc, Adverum Biotech, Alcon, Alkeus, ANI Pharmaceuticals, Annexon, Apellis, Astellas, Bausch and Lomb, Beacon, Biocryst, Boehringer Ingelheim, Celltrion, Cencora, Clearside Biomedical, EyePoint Pharma, Genentech, Glaukos, Kodiak Sciences, Harrow, Janssen, Neurotech, Ocular Therapeutix, Oculis, Opthea, Outlook Therapeutics, Palatin Technologies, Regeneron, RegenxBio, RetinAI, RevOpsis Therapeutics, Roche, Sanofi, Stealth Biotherapeutics, Surrozen; Research: 4DMT, Adverum Biotech, Annexon Biosciences, Astellas, Beacon, Boehringer Ingelheim, Clearside Biomedical, EyeBio, EyePoint Pharma, Genentech, Glaukos, Kanghong/Vanotech, Kodiak Sciences, Ocular Therapeutix, Oculis, Opthea, Perceive Bio, Regeneron, RegenxBio, Roche, Sanofi, Stealth Biotherapeutics; Speaker: Alcon, ANI Pharmaceuticals, Apellis, Astellas, Genentech, Regeneron; Stock/Stock Options: NeuBase, Oxurion, RevOpsis Therapeutics.
Running Title:
Intraoperative hypotension and ocular outcomes.
References
- Lee S, Islam N, Ladha KS, et al. Intraoperative Hypotension in Patients Having Major Noncardiac Surgery Under General Anesthesia: A Systematic Review of Blood Pressure Optimization Strategies. Anesth Analg. 141(2025): 38-60.
- Cònsol G, Moles A, Ricart-Jané D, et al. An in-situ perfusion protocol of rat epididymal adipose tissue useful in metabolic studies. Journal of Lipid Research. 46 (2005): 1803-1808.
- Kouz K, Hoppe P, Briesenick L, et al. Intraoperative hypotension: Pathophysiology, clinical relevance, and therapeutic approaches. Indian J Anaesth. 64 (2020): 90-96.
- Gregory A, Stapelfeldt WH, Khanna AK, et al. Intraoperative hypotension is associated with adverse clinical outcomes after noncardiac surgery. Anesthesia & Analgesia. 132 (2020): 1654-1665.
- Dogan L, Serap Aktas Yildirim, Zeynep Tuğçe Sarıkaya, et al. Different Types of Intraoperative Hypotension and their Association with Post-Anesthesia Care Unit Recovery. Global heart. 18 (2023).
- Harris A. Regulation of retinal and optic nerve blood flow. Archives of Ophthalmology. 116 (1998):1491.
- Jammal AA, Berchuck SI, Mariottoni EB, et al. Blood Pressure and Glaucomatous Progression in a Large Clinical Population. Ophthalmology. 129 (2022): 161-170.
- Stein JD, Khawaja AP, Weizer JS. Glaucoma in Adults–Screening, Diagnosis, and Management. JAMA. 325 (2021): 164.
- Baig MN, Lubow M, Immesoete P, et al. Vision loss after spine surgery: review of the literature and recommendations. Neurosurgical Focus FOC. 23 (2007): E15.
- Kim YS, Han NR, Seo KH. Changes of intraocular pressure and ocular perfusion pressure during controlled hypotension in patients undergoing arthroscopic shoulder surgery. Medicine. 98 (2019): e15461.
- Naderi S. Postoperative visual loss after spine surgery and the role of the neurosurgeon. World Neurosurgery. 86 (2015): 54-55.
- Wijnberge M, Schenk J, Bulle E, et al. Association of intraoperative hypotension with postoperative morbidity and mortality: systematic review and meta-analysis. BJS Open. 5 (2021).
- Stefánsson E, Pedersen DB, Jensen PK, et al. Optic nerve oxygenation. Progress in Retinal and Eye Research. 24 (2004): 307-332.
- Atkins EJ, Newman NJ, Biousse V. Lesions of the optic nerve. Handbook of Clinical Neurology. Published online (2011): 159-184.
- Wright WS, Eshaq RS, Lee M, Kaur G, Harris NR. Retinal Physiology and Circulation: Effect of Diabetes. Comprehensive Physiology. 10 (2020): 933-974.


 Impact Factor:
* 1.2
Impact Factor:
* 1.2
 Acceptance Rate:
79.45%
Acceptance Rate:
79.45%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks

