Intra-articular Tophaceous Gout Mimicking Cruciate Ligament Pathology: Arthroscopic Diagnosis of a Rare Knee Pathology and Comprehensive Review of Literature
Sunil Khemka, Pritam Agrawal, Pradeep Patel*, Ambrish Verma, Ram Khemka
Department of Orthopedics, Shree Narayana Hospital, Raipur, Chhattisgarh, India
*Corresponding Author: Dr Pradeep Patel, MS ORTHO, Department of Orthopedics, Shree Narayana Hospital Raipur, Chhattisgarh, 492001, India.
Received: 07 March 2026; Accepted: 16 March 2026; Published: 23 March 2026
Article Information
Citation: Sunil Khemka, Pritam Agrawal, Pradeep Patel, Ambrish Verma, Ram Khemka. Intra-articular Tophaceous Gout Mimicking Cruciate Ligament Pathology: Arthroscopic Diagnosis of a Rare Knee Pathology and Comprehensive Review of Literature. Journal of Orthopedics and Sports Medicine. 8 (2026): 116-120.
View / Download Pdf Share at FacebookAbstract
Introduction: Tophaceous gout rarely manifests within intra-articular structures of the knee, and involvement of cruciate ligaments is exceptionally uncommon. Such atypical presentations frequently simulate degenerative or cystic ligament pathology on magnetic resonance imaging (MRI), leading to diagnostic delay and inappropriate preoperative diagnosis.
Case Report: A 30-year-old male with chronic kidney disease and hyperuricemia presented with painful hyperflexion of the knee and difficulty in sitting cross-legged. Clinical examination revealed stable Lachman with a doubtful end point, negative anterior and posterior drawer tests, and absence of joint line tenderness. MRI suggested mucoid degeneration of the anterior cruciate ligament. Diagnostic arthroscopy revealed extensive chalky white tophaceous deposits diffusely involving the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), synovium, and articular cartilage. Arthroscopic debridement and debulking were performed. The patient experienced significant pain relief postoperatively and regained comfortable cross-legged sitting by 15 days.
Conclusion: Intra-articular tophaceous gout involving cruciate ligaments is a rare diagnostic masquerader. Arthroscopy remains the definitive diagnostic and therapeutic modality. Gout should be considered in patients with atypical intra-articular knee pathology, especially in the presence of hyperuricemia and renal disease.
Keywords
Tophaceous gout; Anterior cruciate ligament; Posterior cruciate ligament; Mucoid degeneration; Hyperuricemia
Article Details
1. Introduction
Gout is a systemic metabolic disorder resulting from sustained hyperuricemia and subsequent deposition of monosodium urate crystals in joints and periarticular tissues. While the disease classically affects peripheral joints, deep intra-articular involvement of the knee is uncommon, and ligamentous deposition is particularly rare [1-3]. The increasing availability of MRI has led to more frequent detection of atypical intra-articular lesions, many of which are labeled as mucoid degeneration of the ACL, ganglion cysts, synovial proliferative disorders, or intra-articular tumors. Tophaceous gout may radiologically mimic each of these conditions, often resulting in misdiagnosis and delayed definitive treatment [2-4]. Isolated reports have documented gouty tophi within the ACL [1,2,5], PCL [3,6], meniscus [7], synovium and cartilage [8,9], and intraosseous regions of the knee [10]. However, diffuse involvement of both cruciate ligaments and articular cartilage in a young patient remains exceptionally rare. This report presents such a case and provides a comprehensive literature-based discussion of diagnostic challenges, pathophysiology, imaging pitfalls, and management strategies (Figure 1 A,B).
2. Case Report
A 30-year-old male presented with insidious onset knee pain, predominantly during hyperflexion, and progressive difficulty in sitting cross-legged over several months. There was no history of trauma, locking, giving way, or acute inflammatory episodes. The patient was a known case of chronic kidney disease and had persistently elevated serum uric acid levels.
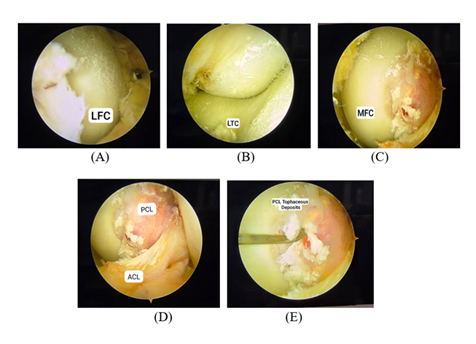
(A) Arthroscopic image of the lateral femoral condyle (LFC) showing granular white tophaceous deposits adherent to the articular cartilage. (B) Arthroscopic view of the lateral tibial condyle (LTC) demonstrating fine chalky urate crystal deposition over the cartilage surface. (C) Arthroscopic visualization of the medial femoral condyle (MFC) demonstrating patchy chalk-like monosodium urate crystal accumulation over the cartilage surface. (D) Arthroscopic view of the posterior cruciate ligament (PCL) showing fluffy white tophaceous deposits attached to the ligament fibers. (E) Intercondylar notch view demonstrating simultaneous involvement of both anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) with surrounding intra-articular tophaceous material.
On examination, the knee demonstrated full range of motion with pain at terminal flexion. Lachman test was stable but with a doubtful end point, whereas anterior and posterior drawer tests were negative. The joint line was non-tender and no effusion was appreciated.
MRI revealed a bulky ACL with intraligamentous increased signal intensity suggestive of mucoid degeneration. The PCL appeared mildly thickened (Figure 1 A,B). Based on these findings, arthroscopic decompression of mucoid ACL was planned.
Diagnostic arthroscopy revealed extensive chalky white, granular tophaceous deposits diffusely involving the ACL, PCL, synovium, and articular cartilage, producing a characteristic “snowstorm” appearance. Whitish granular layering was noted over the femoral condyles and tibial plateau (Figure 2 A-E). Arthroscopic debridement and debulking of tophaceous material from both cruciate ligaments and articular cartilage were performed.
Postoperatively, the patient reported marked pain relief from postoperative day 1. At 15-day follow-up, he was able to sit cross-legged comfortably and achieve painless deep flexion (Figure 3 A,B). The patient was referred for optimization of urate-lowering therapy and management of renal disease.
3. Discussion
Tophaceous gout represents the chronic phase of gout, characterized by organized deposits of monosodium urate (MSU) crystals surrounded by granulomatous inflammation. While acute gout frequently involves the knee joint, chronic intra-articular tophaceous deposition affecting deep ligamentous structures is distinctly uncommon and often under-recognized [1–3]. The available literature is limited to isolated case reports and small series describing involvement of the ACL [1,2,5], PCL [3,6], meniscus [7], synovium and cartilage [8,9], and intraosseous regions of the knee [10]. The present case extends this spectrum by demonstrating diffuse involvement of both cruciate ligaments and articular cartilage in a young patient, initially misinterpreted on MRI as mucoid degeneration of the ACL.
The epidemiology of ligamentous gout is not well defined due to the rarity of reported cases. Most published cases involve middle-aged to elderly patients with long-standing hyperuricemia, renal dysfunction, or metabolic syndrome [2,3,6]. Chronic kidney disease is a particularly strong risk factor due to impaired renal urate excretion, resulting in persistent hyperuricemia and accelerated tophus formation [8,11]. Although tophaceous gout is traditionally associated with prolonged disease duration, recent reports indicate that aggressive tophus formation may occur earlier in patients with renal disease or those receiving diuretics or cyclosporine [8]. The young age of the patient in the present case highlights that ligamentous tophaceous deposition can occur early in the disease course when strong metabolic risk factors are present.
MSU crystal deposition is governed by urate supersaturation and local tissue conditions. Ligaments and fibrocartilaginous structures possess relatively poor vascularity and lower metabolic turnover, potentially favoring crystal deposition and persistence [1,2]. Repetitive microtrauma, mechanical stress, and local hypoxia may further promote deposition and inflammatory response. Histologically, tophi consist of MSU crystal aggregates surrounded by macrophages, foreign body giant cells, and fibroblasts, leading to progressive enlargement and infiltration of adjacent structures. Intra-articular tophi may infiltrate ligament fibers, resulting in ligament thickening and loss of normal architecture, thereby mimicking mucoid degeneration on imaging and occasionally contributing to subtle instability or mechanical restriction [2,3].
Patients with intra-articular tophaceous gout of the knee often present with non-specific symptoms such as chronic pain, stiffness, recurrent effusion, mechanical restriction of motion, or painful hyperflexion, rather than classic acute gouty flares [2,3,8]. Mechanical symptoms such as painful deep flexion or difficulty in sitting cross-legged, as observed in the present case, may result from bulky tophaceous deposits within the intercondylar notch or posterior compartment. The absence of overt inflammatory signs and the presence of apparently stable ligamentous examination may further mislead clinicians toward degenerative or cystic ligament pathology. This atypical presentation contributes to diagnostic delay and highlights the importance of considering gout in the differential diagnosis of unexplained intra-articular knee pathology, particularly in patients with metabolic risk factors.
MRI remains the primary imaging modality for evaluating intra-articular knee lesions; however, the imaging appearance of tophaceous gout is notoriously heterogeneous and non-specific. Tophaceous deposits may appear as low-to-intermediate signal intensity on T1-weighted sequences and variable signal on T2-weighted images depending on crystal density, calcification, and surrounding inflammatory tissue [2,4]. Enhancement patterns following contrast administration are variable and may mimic synovial proliferative disorders. Consequently, lesions are frequently misinterpreted as mucoid degeneration of the ACL, ganglion cysts, pigmented villonodular synovitis, synovial chondromatosis, or even neoplastic processes [2–4]. Similar misinterpretations were reported in cases of ACL and PCL tophi described by Curd et al. and Satti et al. [2,3]. Several intra-articular pathologies of the knee can present with similar MRI findings, making preoperative diagnosis challenging. In particular, tophaceous gout involving the cruciate ligaments may closely mimic mucoid degeneration of the anterior cruciate ligament on imaging. A comparison of the key clinical, radiological, and arthroscopic features of these conditions is summarized in Table 1 along with differential diagnosis in Table 2. In the present case, MRI findings initially suggested mucoid degeneration of the ACL; however, arthroscopy revealed extensive chalky white tophaceous deposits involving both cruciate ligaments and articular cartilage, confirming the diagnosis of diffuse intra-articular gout. Dual-energy computed tomography (DECT) has shown promise in detecting MSU crystal deposition in gout; however, its role in deep intra-articular ligamentous involvement remains limited and is not routinely utilized in clinical practice.
|
Feature |
Mucoid Degeneration of ACL |
Tophaceous Gout of ACL/PCL |
|
Clinical presentation |
Posterior knee pain, limited flexion, usually no metabolic disease |
Chronic knee pain, stiffness, often associated with hyperuricemia or CKD |
|
Ligament appearance |
Diffuse thickening of ACL with intact fibers |
Bulky ligament with irregular infiltrative deposits |
|
MRI signal (T1) |
Intermediate signal within ACL |
Low to intermediate signal intensity |
|
MRI signal (T2) |
High signal giving 'celery stalk' appearance |
Heterogeneous signal due to crystal deposition |
|
Associated findings |
No synovial or cartilage deposits |
May show synovial, cartilage, or intra-articular deposits |
|
Arthroscopy |
Yellowish mucoid material within ligament fibers |
Chalky white granular tophaceous deposits ('snowstorm appearance') |
|
Definitive diagnosis |
Histopathology showing mucoid degeneration |
Identification of monosodium urate crystals |
Table 1: MRI Findings: Mucoid ACL Degeneration vs Tophaceous Gout of Cruciate Ligaments.
Arthroscopy provides direct visualization of intra-articular structures and remains the definitive diagnostic modality. The characteristic chalky white, granular, or “snowstorm” appearance of MSU crystal deposits is virtually pathognomonic [2,6,9]. In several reported cases, the diagnosis of gout was established only at arthroscopy following inconclusive imaging [2,3,6]. Histopathological confirmation demonstrates needle-shaped MSU crystals surrounded by granulomatous inflammation and foreign body giant cells; however, crystal dissolution during routine processing may limit histological identification unless polarizing microscopy or alcohol-fixed specimens are used. Nevertheless, the macroscopic arthroscopic appearance in conjunction with clinical context is often sufficient to establish the diagnosis.
|
Condition |
Clinical Features |
MRI Findings |
Arthroscopic Appearance |
Key Differentiating Feature |
|
Tophaceous Gout |
Chronic pain, stiffness, hyperuricemia |
Variable signal, may mimic mass |
Chalky white 'snowstorm' deposits |
Monosodium urate crystals |
|
Mucoid Degeneration of ACL |
Posterior knee pain, limited flexion |
Thickened ACL, 'celery stalk sign' |
Yellow gelatinous material in ACL |
Ligament fibers preserved |
|
PVNS |
Chronic swelling, recurrent effusion |
Low signal (hemosiderin) |
Brown hypertrophic synovium |
Hemosiderin deposition |
|
Synovial Chondromatosis |
Mechanical symptoms, swelling |
Multiple loose bodies |
Cartilaginous nodules |
Calcified nodules |
|
Ganglion Cyst (ACL/PCL) |
Posterior knee pain |
Well-defined cystic lesion |
Clear gelatinous cyst |
True cystic cavity |
|
Intra-articular Tumor |
Progressive pain/swelling |
Solid heterogeneous mass |
Variable |
Histopathology confirms tumor |
Table 2: Differential Diagnosis of Intra-articular Knee Lesions.
Arthroscopic debridement serves both diagnostic and therapeutic purposes. Removal of bulky tophaceous material relieves mechanical obstruction, reduces synovial inflammation, and improves range of motion [2,6,9,10]. Posterior knee arthroscopy may be required for complete excision of PCL tophi, as demonstrated by Alzobi et al. [6]. Care must be taken to preserve ligament integrity during debridement, particularly when deposits infiltrate ligament fibers. In the present case, judicious debulking of ACL and PCL deposits resulted in rapid symptomatic improvement without compromising ligament stability. Arthroscopy is minimally invasive and associated with rapid recovery, making it the preferred surgical approach in most reported cases. Several isolated case reports have described intra-articular tophaceous gout involving different structures of the knee including cruciate ligaments, meniscus, synovium, and bone. A comparison of previously reported cases with the present case is summarized in Table 3. Compared with previously reported cases, our patient demonstrated simultaneous involvement of both cruciate ligaments and articular cartilage, initially mimicking mucoid degeneration of the ACL on MRI, making it a particularly unusual presentation.
Short-term outcomes following arthroscopic debridement of intra-articular tophaceous gout are generally favorable, with most reports describing significant pain relief and improved range of motion [2,6,9,10]. Long-term outcomes, however, are largely dependent on effective metabolic control. Persistent hyperuricemia predisposes to recurrence of tophaceous deposits and progressive joint degeneration. Although long-term follow-up data are limited, recurrence has been reported in patients with poor adherence to urate-lowering therapy [8,11]. Therefore, surgical intervention should be viewed as an adjunct to, rather than a substitute for, comprehensive medical management.
|
Author (Year) |
Structure Involved |
Clinical Presentation |
Imaging Diagnosis |
Treatment |
Outcome |
|
Melloni et al. [1] |
ACL |
Knee pain, mechanical symptoms |
Intra-articular mass |
Arthroscopic excision |
Symptomatic relief |
|
Curd et al. [2] |
ACL |
Chronic knee pain, limited motion |
ACL mass on MRI |
Arthroscopic debridement |
Good recovery |
|
Satti et al. [3] |
PCL |
Knee pain, suspected cyst |
PCL cyst on MRI |
Arthroscopic removal |
Resolution of symptoms |
|
Alzobi et al. [6] |
PCL |
Posterior knee pain |
PCL mass |
Posterior arthroscopy |
Good outcome |
|
Aoki et al. [7] |
Meniscus |
Pain, mechanical symptoms |
Meniscal lesion |
Arthroscopic excision |
Improved symptoms |
|
Goyal et al. [11] |
Synovium / cartilage |
Knee swelling, mass |
Intra-articular lesion |
Arthroscopic removal |
Clinical improvement |
|
Ma et al. [10] |
Intraosseous knee |
Chronic knee pain |
Intraosseous lesion |
Arthroscopic management |
Symptom relief |
|
Present case |
ACL + PCL + cartilage |
Painful hyperflexion, difficulty cross-leg sitting |
Mucoid ACL on MRI |
Arthroscopic debridement |
Early recovery |
Table 3: Previously Reported Cases of Intra-articular Tophaceous Gout of the Knee.
Effective management of gout requires sustained reduction of serum urate levels through pharmacological therapy (e.g., xanthine oxidase inhibitors or uricosuric agents), dietary modification, and management of comorbidities such as renal disease and metabolic syndrome [8]. Patients with chronic kidney disease require careful selection and dosing of urate-lowering agents. Multidisciplinary collaboration between orthopaedic surgeons, rheumatologists, and nephrologists is essential to optimize outcomes and prevent recurrence of intra-articular tophi.
3.1 Proposed Diagnostic and Management Algorithm
Based on the present case and review of literature, a pragmatic approach to suspected intra-articular tophaceous gout of the knee may include:
- • Detailed metabolic history and serum urate evaluation in patients with atypical intra-articular knee lesions.
- • Careful interpretation of MRI findings, recognizing that mucoid degeneration and cystic lesions may represent gouty tophi in the appropriate clinical context [2,3].
- • Early consideration of diagnostic arthroscopy in cases with discordant clinical and imaging findings.
- • Arthroscopic debridement of tophaceous deposits for symptomatic relief and tissue diagnosis.
- • Long-term urate-lowering therapy and management of underlying metabolic disorders to prevent recurrence.
3.2 Implications for Clinical Practice
Awareness of ligamentous and intra-articular gout is crucial for orthopaedic surgeons, sports medicine physicians, and radiologists. Failure to consider gout in the differential diagnosis may lead to inappropriate labeling of lesions as degenerative or neoplastic, potentially resulting in delayed or suboptimal management. Incorporating metabolic evaluation into the assessment of atypical knee lesions can facilitate earlier diagnosis and targeted treatment.
4. Conclusion and Clinical Message
Intra-articular tophaceous gout involving cruciate ligaments is a rare but important differential diagnosis for atypical ligamentous lesions of the knee. Arthroscopy is both diagnostic and therapeutic. Metabolic evaluation and long-term urate-lowering therapy are essential to prevent recurrence.
Conflict of interest
The authors declare that there are no conflicts of interest regarding the publication of this article.
Funding Statement
No funding was received for this study.
Patient Consent
Written informed consent was obtained from the patient for publication and accompanying images.
References
- Melloni P, Valls R, Yuguero M, et al. An unusual case of tophaceous gout involving the anterior cruciate ligament. Arthroscopy 20 (2004): e94-e97.
- Curd ED, Ravichandiran K, Abouali J. Gouty tophus presenting as an anterior cruciate ligament mass in the knee: Case report and brief review of relevant literature. Int J Surg Case Rep 82 (2021): 105920.
- Satti LR, Mootha AK, Bajjangi US, et al. Atypical presentation of gouty tophus as posterior cruciate ligament cyst: A case report. J Orthop Case Rep 13 (2023).
- Abraham VT. Gouty arthritis versus chondrocalcinosis in a stiff knee. J Orthop Case Rep 16 (2026).
- Gathani H, Jawale S, Samantaray SS, et al. Arthroscopic Treatment of Isolated Tophaceous Gout of the Knee: A Rare Case Report. J Orthop Case Rep 15 (2025): 33-36.
- Alzobi O, Mohammed A, Hantouly A, et al. Tophaceous gout presented as a posterior cruciate ligament mass and addressed by posterior knee arthroscopy. J Orthop Rep (2023): 100275.
- Aoki T, Tensho K, Kato H, et al. Intrameniscal gouty tophi in the knee. JBJS Case Connect 5 (2015): e75.
- Ishida N, Sekiguchi I. Intra-articular mass of the knee by gout tophus: A case report. J Clin Diagn Res 14 (2020): RD01-RD03.
- Sai Krishna M, Chaitanya Reddy YK, Govardhana Reddy G. Arthroscopic image of tophaceous gout of the knee. Int J Orthop Sci 9 (2023).
- Ma YJ, Hsu YP, Wang CY. Arthroscopic management of intraosseous tophaceous gout of the knee: A case report and review of the literature. Formosan Journal of Musculoskeletal Disorders 15 (2024): 120-124.
- Goyal A. Intra-articular mass of the knee by gout tophus: A case report. Journal of Clinical and Diagnostic Research. 2020;14(9): RD01–RD03. doi:10.7860/JCDR/2020/45521.14240.




 Impact Factor:
* 5.3
Impact Factor:
* 5.3
 Acceptance Rate:
73.64%
Acceptance Rate:
73.64%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
