Presenting Features and Short-Term Outcomes of Paraquat Poisoning in a Tertiary Care Hospital of Bangladesh
Dr. Mohammad Omar Faruque Miah*,1, Dr. Fahima Akter Dowel2, Dr. Muhammad Shahidullah3, Dr. Choman Abdullah Mohana4
1Associate Professor, Department of Nephrology, Mymensingh Medical College & Hospital, Mymensingh, Bangladesh
2Senior Medical Officer, Institute of Nuclear Medicine and Allied Sciences (INMAS), Mymensingh, BAEC, Bangladesh
3Associate Professor, Department of Medicine, Mymensingh Medical College & Hospital, Mymensingh, Bangladesh
4Assistant Professor, Department of Endocrinology, Mymensingh Medical College & Hospital, Mymensingh, Bangladesh
*Corresponding Author: Dr. Mohammad Omar Faruque Miah, Associate Professor, Department of Nephrology, Mymensingh Medical College & Hospital, Mymensingh, Bangladesh.
Received: 06 March 2026; Accepted: 16 March 2026; Published: 30 March 2026
Article Information
Citation: Dr. Mohammad Omar Faruque Miah, Dr. Fahima Akter Dowel, Dr. Muhammad Shahidullah, Dr. Choman Abdullah Mohana. Presenting Features and Short-Term Outcomes of Paraquat Poisoning in a Tertiary Care Hospital of Bangladesh. Fortune Journal of Health Sciences. 9 (2026): 156-161.
View / Download Pdf Share at FacebookAbstract
Background: Paraquat poisoning is a major cause of pesticide-related morbidity and poor clinical outcomes in low- and middle-income countries. Data from Bangladesh is still scarce. This study was conducted to evaluate clinical features, renal involvement, and short-term outcomes of paraquat poisoning and compare findings with existing literature.
Methods: This prospective observational study was conducted from January to July 2023 at Mymensingh Medical College Hospital. Fifty-four patients with confirmed paraquat ingestion were enrolled. Clinical features, laboratory findings, renal outcomes, and five-week outcomes were analyzed.
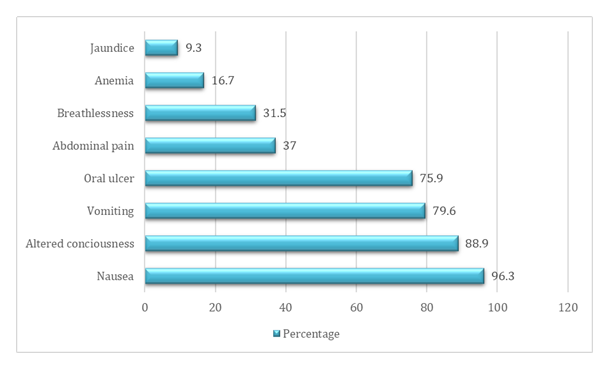
Findings: The mean age was 21.98 ± 8.85 years, with male predominance (61.1%). Most patients presented within 24 hours (77.8%). Common features included nausea (96.3%), altered consciousness (88.9%). vomiting (79.6%) and oral ulceration (75.9%), Renal failure developed in 72.2% of patients, and 35.2% required hemodialysis. The overall mortality rate was 57.4%.
Conclusion: Owing to its continued availability and severe outcomes, paraquat poisoning represents a significant public health problem, highlighting the dire need for preventive strategies, regulatory control, and standardized management guidelines.
Keywords
Paraquat poisoning; agricultural pesticide; clinical features; short-term outcomes; acute renal failure; toxicity
Article Details
Introduction
Paraquat is a highly effective, non-selective, and fast-acting herbicide that remains widely used in agriculture worldwide. Owing to its pronounced acute toxicity, even minimal ingestion or dermal exposure can result in severe systemic injury, necessitating specialized handling, protective equipment and training. [1] Despite being banned or strictly regulated in more than 67 countries because of its high toxicity and the absence of a specific antidote, paraquat continues to be used extensively, particularly in South-east Asia and Pacific regions, largely due to its low cost and agricultural efficiency. [2]
Paraquat toxicity predominantly involves the lungs, kidneys, liver, and gastrointestinal tract. Following ingestion, the compound is actively concentrated in pulmonary tissue via the polyamine transport system, where it generates reactive oxygen species (ROS) through redox cycling. This process leads to lipid peroxidation, alveolar epithelial damage and progressive pulmonary fibrosis. Concurrent oxidative stress and systemic inflammation contribute to subsequent renal and hepatic dysfunction. [3]
The World Health Organization (WHO) lists paraquat as a Class II moderately hazardous pesticide and Pesticide Action Network International as a highly hazardous pesticide. [4] Ingestion of very minute amounts ultimately leads to development of acute multi-organ failure, even death. [5] Mortality rate is 60–80% across the planet; about 20 deaths per million individuals worldwide take place as a result of acute paraquat poisoning. [4-5]
The diagnosis is largely clinical, based on the history of exposure and presenting features. Laboratory confirmation includes urine dithionite test or plasma paraquat level measurement, although availability of these tests is limited in resource-constrained settings. Coming to the treatment, there are no standard guidelines for the management of this condition as of now. Interventions include preventing paraquat absorption with activated charcoal or gastric lavage, increasing paraquat elimination by hemodialysis and administering glucocorticoids, immunosuppressants and antioxidants. However, this approach does not provide remarkable benefits in preventing the toxicities of paraquat. [3]
Despite all, paraquat is readily available in agrochemical shops under various trade names and often used without proper personal protective equipment (PPE) in Bangladesh. It is a major cause of poisoning-related hospital admissions, particularly in rural regions, where intentional self-poisoning is a common mode of exposure. A retrospective analysis conducted at the Dhaka Medical College Hospital (DMCH) reported that paraquat was responsible for up to 13.6% of all pesticide poisoning cases, with a case fatality rate exceeding 70%. [6] Another study in Chattogram Medical College Hospital discovered similar findings, where most victims were young adults (aged 15–30) and had ingested the poison with suicidal intent. [7]
Studies confirm that banning or severely restricting paraquat directly leads to a significant decline in suicide rates and fatal, often impulsive, poisoning cases. [1] However, the continued, widespread use of paraquat highlights significant gaps in global pesticide regulation, mental health support and agricultural safety practices. The persistent use can be linked to several factors such as weak enforcements of regulations, lack of competitive alternatives, ineffective restrictions and lack in training. [1]
There is dearth of published literature on paraquat poisoning in Bangladesh as it is grossly under-reported, as well as the true burden is not well-documented. Therefore, the aim of this study was to evaluate the clinical presentations and short-term outcomes of the patients.
Methods
Study design
This was a prospective observational study conducted over a six-month period from January 2023 to July 2023.
Study setting
The study was carried out in the Departments of Nephrology and Medicine at Mymensingh Medical College Hospital (MMCH), a tertiary care referral center in Bangladesh.
Study population and sample size
A total of 54 patients with a confirmed history of paraquat ingestion were enrolled in the study. The sample size was determined based on real-world case availability during the study period.
Sampling technique
Purposive consecutive sampling was employed, whereby all eligible patients presenting during the study period were included until the desired sample size was reached.
Eligibility criteria
Patients with a confirmed history of paraquat ingestion within the preceding seven days were included and patients who declined to provide informed consent were excluded from the study.
Data collection procedure
Demographic information and clinical data were collected using a standardized data collection sheet at the time of admission. Clinical evaluation focused on gastrointestinal, renal, hepatic, and respiratory manifestations.
Blood (3 mL) and urine (10 mL) samples were obtained for laboratory investigations. The following tests were performed:
- • Complete blood count (CBC)
- • Random blood sugar (RBS)
- • Serum creatinine
- • Serum alanine aminotransferase (ALT)
- • Serum electrolytes (sodium, potassium, chloride)
- • Urine routine microscopic examination (RME)
Additional investigations included chest X-ray (CXR) and electrocardiogram (ECG), as clinically indicated.
Follow-up and outcome assessment
Patients were followed for a period of up to five weeks following ingestion. Outcomes were assessed in terms of clinical recovery or adverse outcome during the follow-up period. The need for renal replacement therapy, including hemodialysis, was recorded.
Ethics
The study was conducted in accordance with the ethical principles outlined in the Declaration of Helsinki. Ethical approval was obtained from the Institutional Review Board (IRB) of MMCH prior to commencement of the study. Written informed consent was obtained from all participants or their legally authorized guardians before enrollment. Confidentiality of patient information was strictly maintained throughout the study. Personal identifiers were removed from the data collection forms and all clinical data were used solely for research purposes. Participation in the study was voluntary, and patients were informed of their right to withdraw from the study at any stage without any impact on their standard medical care.
Results
Table 1: Baseline characteristics of the participants [n=54]
|
Attributes |
Values |
|
Age (in years) [Mean ± SD] |
21.98 ± 8.85 |
|
Gender [n/%] |
|
|
Male |
33 (61.1) |
|
Female |
21 (38.9) |
|
Most common area of residence [n/%] |
|
|
Mymensingh |
31 (57.4) |
|
Timing of hospitalization after ingestion [n/%] |
|
|
Within 24 hours |
42 (77.8) |
|
After 24 hours |
12 (22.2) |
Mean age of the respondents was 21.98 ± 8.85 years and majority of them were males [33, 61.1%]. A significant proportion of patients (57.4%) hailed from Mymensingh. Lastly, maximum patients [42, 77.8%] were brought to the hospital within 24 hours of accidental/intentional ingestion. (Table 1).
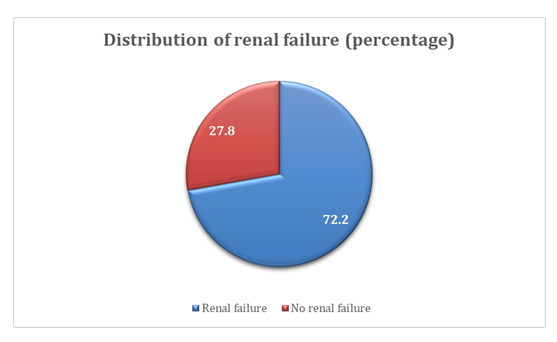
Concerning renal outcomes, majority of the patients [72.2%] developed renal failure after ingestion of paraquat. (Figure 2).
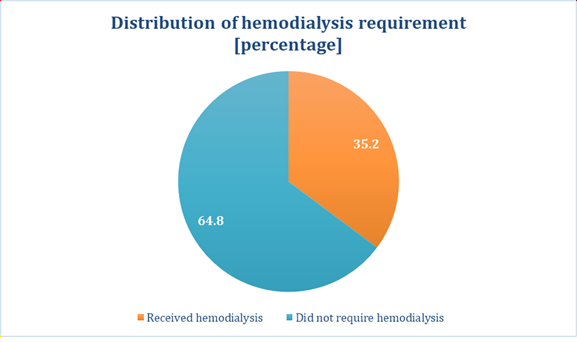
Regarding requirement of hemodialysis of the patients, it is clearly evident that approximately one-third patients [35.2%] received hemodialysis treatment. (Figure 3).
Table 2: Laboratory findings of the study subjects [n=54]
|
Parameter |
Mean value |
|
Hemoglobin (g/dL) |
12.88 |
|
Random blood sugar (mmol/L) |
5.65 |
|
Serum creatinine (mg/dL) |
4.31 |
|
Serum alanine aminotransferase (IU/L) |
70.4 |
|
Serum sodium (mmol/L) |
138.09 |
|
Serum potassium (mmol/L) |
3.99 |
|
Serum chloride (mmol/L) |
101.73 |
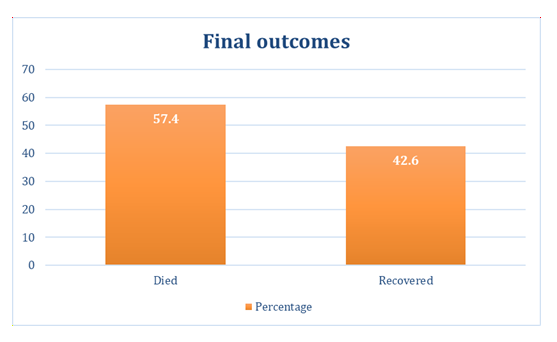
It is visible that, mean serum creatinine level was highly elevated in the patients [4.31 mg/dL]. Also, mean S. alanine aminotransferase was mildly raised [70.4 IU/L] Other tests such as hemoglobin, blood sugar and serum electrolytes were mostly within the normal range. (Table 2). Lastly, it was found that, the majority of the patients [57.4%] could not survive despite hospital admission. (Figure 4).
Discussion
This prospective observational study describes the clinical characteristics, renal involvement, and short-term outcomes of paraquat poisoning in a tertiary care hospital in Bangladesh.
The mean age of patients in this study was 21.98 ± 8.85 years, with the majority below 30 years of age. This is comparable to findings reported from Sri Lanka, India, and China, where paraquat poisoning predominantly affects young adults aged 15–30 years. [8] Gawarammana et al. and Wilks et al. reported similar age distributions, attributing this pattern to impulsive ingestion and easy access to agricultural pesticides among younger populations. [9-10]
Male predominance (61.1%) observed in this cohort is consistent with studies from South Asia and Southeast Asia, where males account for 55–70% of paraquat poisoning cases. This has been linked to greater occupational exposure and higher prevalence of pesticide use among males in agricultural communities. [11]
In the present study, 77.8% of patients presented within 24 hours of ingestion. This rate of early presentation is higher than that reported in several regional studies, where delayed presentation beyond 24 hours ranged from 35% to 50%. Despite earlier hospital arrival in this cohort, outcomes remained poor, suggesting that early presentation alone may not significantly alter prognosis in the absence of effective antidotal or extracorporeal detoxification therapies. [8]
Gastrointestinal manifestations were the most frequent presenting symptoms, with nausea (96.3%), altered conciousness (88.9%), vomiting (79.6%), and oral ulceration (75.9%). Relevant literature reported vomiting and loss of consciousness to be the outstanding clinical features. [11] In another paper by Oghabian et al. it was found that, oral ulceration, respiratory distress and excessive salivation were the most commonly encountered features among the paraquat poisoning cases. [12]
Renal failure occurred in 72.2% of patients, confirming the kidney as a major target organ in paraquat toxicity. This incidence is consistent with existing literature, where acute kidney injury rates ranged from 60% to 80%. [13] The mean serum creatinine level of 4.31 mg/dL in this study is comparable to values reported in regional and worldwide context, indicating substantial nephrotoxicity. [14]
Hemodialysis was required in 35.2% of patients. Similar proportions have been reported in regional studies; however, multiple authors have demonstrated that conventional hemodialysis does not significantly improve survival unless combined with early hemoperfusion. [15]
Aside from elevated serum creatinine and mild transaminase elevation, most laboratory parameters were within normal limits. Comparable biochemical patterns have been reported in prior studies, where renal and hepatic markers were the most consistently affected laboratory variables. Electrolyte disturbances were not prominent in this cohort, consistent with findings from several hospital-based series where abnormalities were largely secondary to vomiting or renal dysfunction rather than direct toxicity. [8, 11]
Paraquat damages the heart, kidneys, liver, adrenal glands, central nervous system, muscles and spleen causing multiple organ failure. Several literature associated paraquat poisoning with acute lung injury, pulmonary hypertension, leukocytosis, metabolic acidosis, enlarged heart, acute kidney injury, generalized edema and increased level of amylase, glucose and creatinine. [16]
The mortality rate in this study was 57.4%, which falls within the range reported internationally (40–70%). Similar fatality rates have been reported in hospital-based studies from Bangladesh, India, and China. [17] An important finding reported was that, mortality correlates with blood plasma levels, with levels >0.2mg/mL at 24 hours often being fatal. Studies from countries that have implemented national bans on paraquat, such as Sri Lanka and South Korea, have demonstrated a marked reduction in poisoning-related deaths, highlighting the importance of regulatory interventions rather than reliance on clinical management alone. [18-21]
This study has several limitations. First, it was a single-center study with a relatively small sample size, which may limit the generalizability of the findings. Second, detailed information regarding patients’ mental health status, psychosocial stressors, and intent of ingestion was not systematically assessed, precluding analysis of underlying behavioral and psychiatric risk factors. Third, quantitative confirmation of paraquat exposure using plasma paraquat levels or urine dithionite testing was not available, and diagnosis relied primarily on clinical history. Finally, follow-up was restricted to five weeks, and long-term complications, particularly chronic pulmonary and renal sequelae, could not be assessed.
Conclusion
The present study demonstrates that paraquat poisoning predominantly affects young adults and is associated with severe multisystem involvement, particularly acute renal failure. Despite early hospital presentation in most cases, short-term outcomes remain poor, with high mortality rates. These findings reinforce the need for stricter regulatory control of paraquat, improved access to advanced supportive therapies, and the development of standardized national management guidelines.
Conflict of interest
The authors disclose no conflict of interest.
References
- Utyasheva L, Amarasinghe P, Eddleston M. Paraquat at 63—the story of a controversial herbicide and its regulations: It is time to put people and public health first when regulating paraquat. BMC Public Health 25 (2025): 3089.
- Bromilow RH. Paraquat and sustainable agriculture. Pest Management Science: formerly Pesticide Science 60 (2004): 340-9.
- Shabrina LS, Ahmad A, Fadrian F. Diagnosis and management of paraquat intoxication.
- Kotal S, Chatterjee S, Pain S, et al. A prospective study to assess the profile and outcome of acute paraquat poisoning in a tertiary care hospital of West Bengal. Indian Journal of Critical Care Medicine: Peer-reviewed, Official Publication of Indian Society of Critical Care Medicine 18 (2025): 678.
- Ko DR, Chung SP, You JS, et al. Effects of paraquat ban on herbicide poisoning-related mortality. Yonsei medical journal 58 (2017): 859.
- Rahman AF, Al Kafi S, Naiem Z. Study on Clinical Profile and Treatment Outcome of Acute Paraquat Poisoning in an Intensive Care Unit in Bangladesh. Journal of Medicine 25 (2024): 129-35.
- Parvin R, Hasan MK, Sarkar P, et al. Fatal Paraquat Poisoning in a 15-Year-Old Girl. Journal of Enam Medical College 7 (2017): 107-10.
- Goyal P, Gautam PL, Sharma S, et al. A study of paraquat poisoning presentation, severity, management and outcome in a tertiary care hospital: Is there a silver lining in the dark clouds?. Indian Journal of Critical Care Medicine: Peer-reviewed, Official Publication of Indian Society of Critical Care Medicine 28 (2024): 741.
- Gawarammana I, Buckley NA, Mohamed F, et al. High-dose immunosuppression to prevent death after paraquat self-poisoning–a randomised controlled trial. Clinical toxicology 56 (2018): 633-9.
- Wilks MF, Fernando R, Ariyananda PL, et al. Improvement in survival after paraquat ingestion following introduction of a new formulation in Sri Lanka. PLoS medicine 5 (2008): e49.
- Delirrad M, Majidi M, Boushehri B. Clinical features and prognosis of paraquat poisoning: a review of 41 cases. International journal of clinical and experimental medicine 8 (2015): 8122.
- Oghabian Z, Williams J, Mohajeri M, et al. Clinical features, treatment, prognosis, and mortality in paraquat poisonings: a hospital-based study in Iran. Journal of research in pharmacy practice 8 (2019): 129-36.
- Asl AS, Dadashzadeh P. Acute kidney injury in patients with paraquat intoxication; a case report and review of the literature. Journal of Renal Injury Prevention 5 (2016): 203.
- Das A, Neera NS, Chowdhury FU, Kahhar MA. Acute lung fibrosis following paraquat poisoning. Bangladesh Journal of Medicine 29 (2018): 41-4.
- Eizadi-Mood N, Jaberi D, Barouti Z, et al. The efficacy of hemodialysis on paraquat poisoning mortality: a systematic review and meta-analysis. Journal of research in medical sciences 27 (2022): 74.
- Tan JT, Letchuman Ramanathan GR, Choy MP, et al. Paraquat poisoning: experience in hospital taiping (year 2008-october 2011). Med J Malaysia 68 (2013): 384-8.
- Tarafder P, Iqbal MA, Hossain MM. Clinical Profile and Mortality Patterns in Acute Paraquat Poisoning: A Retrospective Observational Study in a Tertiary Care Hospital. Barind Medical College Journal 11 (2025): 175-9.
- Cha ES, Chang SS, Gunnell D, et al. Impact of paraquat regulation on suicide in South Korea. International journal of epidemiology 45 (2016): 470-9.
- Sen I, Bhadury S, Roy D. Paraquat Poisoning Presenting as Sinus Bradycardia; A Rare Clinical Manifestation. Indian Journal of Forensic Medicine & Toxicology 19 (2025).
- Buckley NA, Fahim M, Raubenheimer J, et al. Case fatality of agricultural pesticides after self-poisoning in Sri Lanka: a prospective cohort study. The Lancet global health 9 (2021): e854-62.
- Ravichandran R, Amalnath D, Shaha KK, et al. Paraquat poisoning: A retrospective study of 55 patients from a tertiary care center in Southern India. Indian Journal of Critical Care Medicine: Peer-reviewed, Official Publication of Indian Society of Critical Care Medicine 24 (2020): 155


 Impact Factor:
* 6.2
Impact Factor:
* 6.2
 Acceptance Rate:
76.33%
Acceptance Rate:
76.33%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
