Ultrasound Guided MTP Aspiration and Injection in the Emergency Department: A Case Series
Scott C Everett MD1*, Nathanael J Garcia MD1, Katherine E Hayman MD2, Casey M Glass MD1,3, Nicole J Prendergast MD1,2
1Department of Emergency Medicine, Atrium Health Wake Forest Baptist Medical Center, 1 Medical Center Blvd, Winston-Salem, North Carolina, 27157, USA
2Department of Sports Medicine, Atrium Health Wake Forest Baptist Medical Center, 1 Medical Center Blvd, Winston-Salem, North Carolina, 27157, USA
3Department of Ultrasound Medicine, Atrium Health Wake Forest Baptist Medical Center, 1 Medical Center Blvd, Winston-Salem, North Carolina, 27157, USA
*Corresponding Author: Scott C Everett MD, Department of Emergency Medicine, Atrium Health Wake Forest Baptist Medical Center, D 1 Medical Center Blvd, Winston-Salem, North Carolina, 27157, USA.
Received: 20 March 2026; Accepted: 26 March 2026; Published: 31 March 2026
Article Information
Citation: Scott C Everett, Nathanael J Garcia, Katherine E Hayman, Casey M Glass, Nicole J Prendergast. Ultrasound Guided MTP Aspiration and Injection in the Emergency Department: A Case Series. Journal of Orthopedics and Sports Medicine. 8 (2026): 121-125.
View / Download Pdf Share at FacebookAbstract
Background: Gout is a common presenting complaint in the emergency department. Ultrasound-guided intra-articular corticosteroid injections have been previously described in rheumatology literature for the treatment of acute gout. Emergency medicine providers commonly encounter gout and possess the necessary skill set to treat patients with intra-articular injections. This can be a safe, low-risk, and effective treatment, particularly in patients with contraindications to standard therapy, such as those with renal impairment and other comorbidities.
Case Report: Four patients underwent ultrasound-guided intra-articular steroid injections in the emergency department for the treatment of gout and pseudogout in three metatarsophalangeal joints and one radiocarpal joint. These patients were given injections based on risk factors precluding them from receiving standard oral therapy, their ability to receive oral and injection therapy, or personal preference.
Keywords
Case series; Gout; Pseudogout; MTP; Arthrocentesis
Article Details
1. Introduction
The prevalence of gout and pseudogout are difficult to assess, given the definitive diagnosis requires arthrocentesis. It is estimated that gout affects roughly 12.1 million patients in the US annually [1]. An article in 2022 evaluated the US National Emergency Department Sample and National Inpatient Sample databases from 2019, which identified 196,774 patients that presented to the emergency department (ED) with the primary diagnosis of gout, and of those, 11,485 patients were hospitalized [2]. There is no robust data published on the quantity of ED visits annually for pseudogout with global and domestic prevalence data also lacking.
Gout and pseudogout are two chronic diseases characterized by intra-articular accumulation of monosodium urate crystals and calcium pyrophosphate dihydrate crystals, respectively, which commonly manifest as painful inflammatory arthritis [3]. Diagnosis is often clinical, but the gold standard is synovial fluid analysis [3]. Current management recommendations include oral Nonsteroidal anti-inflammatory drugs (NSAIDs) or colchicine [4]. Steroids are an additional treatment option, which can be delivered orally, intravenously, or intra-articularly [4]. While many patients receive NSAIDs or colchicine for initial therapy, some patients have comorbid conditions such as chronic kidney disease, hepatic dysfunction, diabetes, and severe cardiovascular disease. Unfortunately, patients with these conditions are often not good candidates for oral or systemic therapy with NSAIDs or colchicine. Similarly, systemic steroids are commonly avoided due to adverse effects such as dysphoria, mood disorders, elevation of blood glucose levels, immune suppression, and fluid retention [5].
Meanwhile, intra-articular steroid injections have a greater safety profile given their lack of systemic absorption and have demonstrated efficacy in providing analgesia [6]. Likewise, in the treatment of gout, there is equivocal success both in analgesia and time to analgesia with intra-articular steroids when compared to NSAIDs [7]. With increased disease prevalence and difficulties with PCP access, inflammatory arthritides such as gout and pseudogout continue to be a common presenting complaint to the ED. Given the various comorbidities and ongoing illnesses seen in the ED, many patients are not good candidates for systemic therapy. Despite the effectiveness intra-articular steroid injection, there is no available evidence discussing the use or utility of intra-articular injections for gout and pseudogout in the ED. This is likely related to time constraints and lack of provider familiarity with the necessary techniques. Intra-articular injections under ultrasound (US) guidance are safe and effective in treating gout and should be utilized in the ED for those who cannot use standard of care therapies.
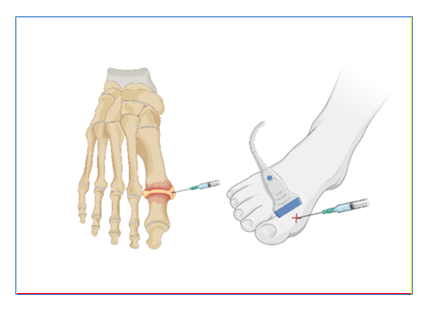
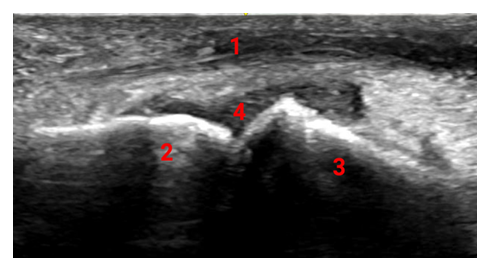
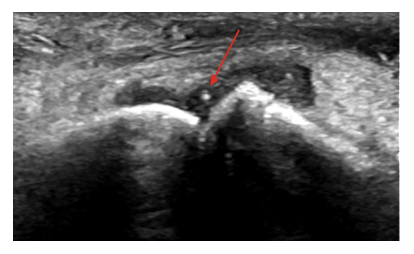
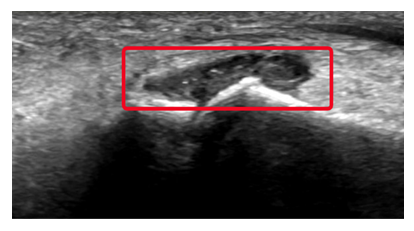
Once the patient has been consented, they are placed in a seated or supine position and instructed to relax their first MTP and if the provider has assistance at bedside, have another provider provide traction to the great toe to help improve joint space visualization. The physician uses sterile gloves and a sterile ultrasound probe cover. The skin is prepped and draped in a sterile fashion. The ultrasound probe is positioned along the long axis of the digit over the metatarsophalangeal (MTP) joint [8]. The probe is positioned parallel to the toe and the extensor hallucis longus (EHL) on the dorsum of the foot as illustrated in Figure 1. The EHL will be visualized on the top of the screen as seen in Figure 2. Next, a topical or local anesthetic is used to anesthetize the skin of the medial aspect of the joint. A 1.5-inch 21–25-gauge needle is inserted into the joint space under US guidance. Once the needle is present in the joint, as seen in Figure 3, aspiration can occur if there is already a joint effusion present. Then, syringes are exchanged sterilely, and joint injection with anesthetic; and corticosteroid can be performed. Visualization of hypoechoic material in the joint capsule, as seen in Figure 4, indicates correct administration into the articular space. After injection, the needle is retracted, and direct pressure is applied to allow for hemostasis [8].
We describe a series of cases in which patients presented to the Emergency Department with significant joint pain and limitation of function. All patients received a steroid joint injection with improvement in symptoms.
2. Case Series
2.1 Patient 1
An 85-year-old male with a history of neuropathy, gout, hypertension, hyperlipidemia, hypothyroidism, and chronic kidney disease (CKD) presented to the ED with a 1-day history of progressive pain in his right great toe. His exam demonstrated mild local erythema and tenderness overlying the first MTP of the right foot. The patient’s X-ray demonstrated mild swelling and moderate degenerative changes at the right MTP without acute fracture or malalignment. A point-of-care US revealed an effusion at the right first MTP. Under US guidance using sterile technique, the joint was aspirated, revealing yellow synovial fluid. Following aspiration, the joint was injected with 1mL 0.5% ropivacaine and 40mg (1mL) triamcinolone acetonide. The aspirate was sent for fluid analysis and demonstrated calcium pyrophosphate crystals, consistent with a diagnosis of pseudogout. The patient experienced relief of his symptoms, and during follow-up call reported that he was back to walking 4 miles per day.
2.2 Patient 2
A 53-year-old male with a history of type II diabetes mellitus, gout, heart failure, chronic obstructive pulmonary disease, chronic lymphedema, and prior deep vein thrombosis on Eliquis presented to the ED for several days of bilateral foot swelling. His exam revealed a small area of erythema over the left MTP, but he had symmetric tenderness of bilateral MTPs. X-rays of both feet were obtained and were unremarkable for any acute fractures or dislocations but did reveal diffuse soft tissue edema bilaterally. US was performed at the bedside and revealed an effusion of the left MTP. Arthrocentesis was performed of the left MTP with resultant uric acid crystals. He received bilateral injections of 1mL 0.5% ropivacaine and 40mg (1mL) triamcinolone acetonide. Follow-up included a podiatry visit 3 days later and a primary care visit 2 weeks later, with improvement noted in both swelling and pain bilaterally.
2.3 Patient 3
A 48-year-old male with heart failure with reduced ejection fraction (HFrEF), hypertension, hyperlipidemia, CKD, polysubstance use, and gout presented to the ED for evaluation of left arm swelling. Physical exam revealed edema and warmth from the midshaft of the left forearm through the hand, with some discomfort on flexion and extension of the wrist. He was afebrile with no leukocytosis and was without significant pain with range of motion, so there was lower concern for septic arthritis. He reported previous gout flares of the wrist. Given the patient’s kidney disease with a baseline GFR in the 30s to 50s, indomethacin and colchicine were deferred as treatment modalities. He was empirically given an injection of 1mL 0.5% ropivacaine and 40mg (1mL) triamcinolone acetonide. The patient followed up 5 days later in clinic with some pain in the radial aspect of the wrist, but his discomfort had improved overall. He was able to move his wrist without difficulty and was able to perform activities of daily living without significant disability.
2.4 Patient 4
A 36-year-old female with a history of gout in her left ankle presented with worsening right great toe pain for one week, with no clear inciting event, and pain resistant to ibuprofen. Her exam revealed tenderness to palpation of the right first MTP joint with overlying swelling. X-ray of the right foot was notable for soft tissue swelling changes with erosive findings raising concern for gout of the first MTP joint. The patient was offered oral medications or a steroid injection and ultimately elected for intra-articular injection of the first MTP joint with 1mL 0.5% ropivacaine and 40mg (1mL) triamcinolone acetonide. The patient had improvement in her symptoms and was able to ambulate without difficulty on follow-up.
3. Discussion
Gout is the most common inflammatory arthritis worldwide [9]. It is driven by a reaction to monosodium urate crystals formed from hyperuricemia in and around joints. Specifically, in the US, 12.1 million adults are affected by gout, an increase from 9.2 million in 2021, with some studies citing prevalence above 5% [1,10]. Gout can be managed in a variety of ways in the ED based on the degree of severity. Simple recommendations such as decreased intake of foods such as certain meats, shellfish, alcohol, purine-rich foods, etc., can be the first step in preventing future gout attacks [11]. Also, it is important to identify causes such as medications like hydrochlorothiazide, which is known to increase uric acid levels. Other management strategies of inflammatory arthropathies in the ED generally consist of a combination of anti-inflammatory medications and steroids. A randomized controlled trial of 120 patients found no difference between oral naproxen and oral prednisolone in the reduction of pain scores at 90 hours [12]. Patients are often given colchicine as well for gout flares, however those with renal or hepatic impairment should not be given colchicine. Patients with renal dysfunction should not be receiving NSAIDs due to the risk of further renal dysfunction [4]. Patients who are unable to utilize common modalities of treatment, such as NSAIDs or colchicine, could be offered intra-articular steroid injections in the ED. These are contraindicated in any patient with confirmed or concern for septic arthritis, but intra-articular steroid injections have been shown to be effective in the treatment of gout and pseudogout, although there is no randomized controlled trial data comparing intra-articular injections to standard therapy [13].
Why an Emergency Physician Should Be Aware of This?
Gout, pseudogout, and other inflammatory arthropathies are painful conditions which result in limitation of patient activity. When these patients present to the ED, consideration should be given to performing arthrocentesis and injection for both confirmation of diagnosis and treatment of these conditions. There is a subset of patients presenting with gout and other inflammatory arthropathies to the ED who are not good candidates for standard therapies, it is imperative that ED providers consider other alternatives to management including ultrasound-guided intraarticular injection which carries a lower risk in these populations. ED providers possess the skills necessary to perform US-guided intra-articular injections in the ED. Emergency medicine providers should consider familiarization with MTP injection techniques given the potential benefit to patients.
References
- FitzGerald JD. Gout. Ann Intern Med 178 (2025).
- Yokose C, McCormick N, Lu N, et al. Nationwide racial/ethnic disparities in US emergency department visits and hospitalizations for gout. Rheumatology 62 (2022): 2247-2251.
- Sidari A, Hill E. Diagnosis and Treatment of Gout and Pseudogout for Everyday Practice. Primary Care: Clinics in Office Practice 45 (2018): 213-236.
- Gout treatment of flares. UpToDate (2026).
- Major adverse effects of systemic glucocorticoids. UpToDate (2026).
- Kang MH, Moon KW, Jeon YH, Cho SW. Sonography of the first metatarsophalangeal joint and sonographically guided intraarticular injection of corticosteroid in acute gout attack. Journal of Clinical Ultrasound 43 (2014): 179-186.
- Randomized Controlled Trials. The Journal of Rheumatology 45 (2017): 128-136.
- Arthrocentesis of the Foot. Internet Book of MSK Ultrasound (2022).
- DML E. Global epidemiology of gout: Prevalence, incidence, treatment patterns and risk factors. Nature Reviews Rheumatology.
- Yip K, Berman J. What Is Gout? JAMA 326 (2021): 2541.
- Hainer BL, Matheson E, Wilkes RT. Diagnosis, treatment, and prevention of gout. American Family Physician 90 (2014): 831-836.
- Janssens HJ, Janssen M, van de Lisdonk EH, et al. Use of oral prednisolone or naproxen for the treatment of gout arthritis: a double-blind, randomised equivalence trial. Lancet 371 (2008): 1854-1860.
- FitzGerald JD, Dalbeth N, Mikuls T, et al. 2020 American College of Rheumatology Guideline for the Management of Gout. Arthritis Care & Research 72 (2020): 744-760.



 Impact Factor:
* 5.3
Impact Factor:
* 5.3
 Acceptance Rate:
73.64%
Acceptance Rate:
73.64%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
